Extensive Choroidal Effusion after Argon Laser Peripheral Iridoplasty: A Case Report
Ali Salehi, Farzan Kian-Ersi, Heshmat Ollah Ghanbari, Samira Ahmadi, Mohammad-Hasan Alemzadeh Ansari
Ali Salehi, Farzan Kian-Ersi, Heshmat Ollah Ghanbari, Samira Ahmadi, Mohammad-Hasan Alemzadeh-Ansari*
Department of Ophthalmology, Isfahan Eye Research Center, Isfahan University of Medical Sciences, Isfahan, Iran
- *Corresponding Author:
- Mohammad-Hasan Alemzadeh-Ansari
Department of Ophthalmology
Isfahan Eye Research Center, Isfahan University of Medical Sciences
Isfahan 81488-95185, Iran
Tel: +98916 607 8735
Email: mh.aansari@gmail.com
Abstract
This report describes a patient extensive chroidal effusion after Argon Laser Peripheral Iridoplasty (ALPI). This 45 year old man reffered with bilateral acute angle closure glaucoma. Nd-YAG laser peripheral iridotomy was successfully performed and IOP was controlled. Ten years after laser peripheral iridotomy, referred again with angle closure glaucoma and ALPI was done. Chroidal effusion developed in right eye one month after ALPI despite high IOP, and resolved completely after corticosteroid therapy. Based on this case report, choroidal effusion appears to be another complication of ALPI.
Keywords
Sudan, Egypt, Israel, Darfur, Refugees, UNHCR, Muatafa Mahmud, Traffickers, Sinai
Introduction
Argon laser peripheral iridoplasty was done for angle closure glaucoma. This procedure has been described safe, but we describe a case that developed choroidal effusion after ALPI.
Case Report
A 45 year old man with maternal history of glaucoma was referred to our emergent department with bilateral acute angle closure glaucoma, 12 years ago. He had no history of blood hypertension or coaglupathy, and the history was negative for eye diseases or treatments. He was hyperopia with a refractional error +4.25 and +6.75 for right and left eye, respectively. At that time, anterior chamber of eyes was shallow and intraocular pressure (IOP) was 40 mmHg and 37 mmHg for right and left eye, respectively. Central corneal thickness was measured 445 and 449 μm for right and left eye, respectively. Gonioscopy revealed bilateral close angle. Nd-YAG laser peripheral iridotomy was successfully performed to both eyes and Latanoprost drop one time daily and Acetazolamide drops three times daily were prescribed.
He was asymptomatic until 2 years ago; his IOP was raised and was not responded to his medications. IOP was 30 mmHg and 22 mmHg for right and left eye, respectively. On fundoscopy, cup to disk ratio was 70% and 19% for right and left eye, respectively. Gonioscopy was done in this visit and showed close angle without peripheral anterior synechia (PAS).
Using the central nonmirrored part of a Goldman lens, argon laser peripheral iridoplasty (ALPI) was performed on both eyes circumferentially at the periphery of the iris, simultaneously. Some 24 laser burns of 0.2 second duration, 500 μm spot-size, and 500 mW were applied to 360° of the angle. Prednisolone 0.5% drops four times daily were prescribed for both eyes for one week following the procedure. The ALPI successfully reduced the pressure to 14 mmHg and 13 mmHg. This level of IOP was maintained for one month. Topical Latanoprost once daily was continued after ALPI. At all visits following ALPI the patient was asymptomatic; IOP was controlled and best corrected visual acuity was 1.0 in both eyes. There was no evidence of a choroidal effusion.
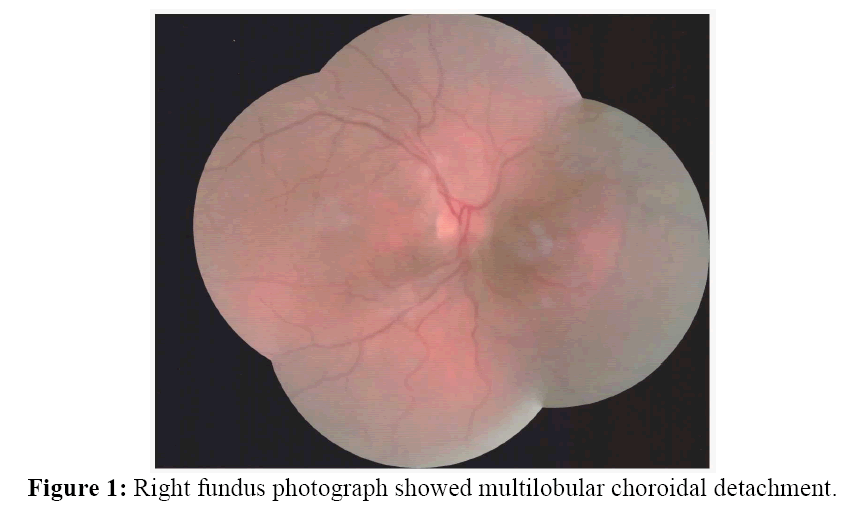
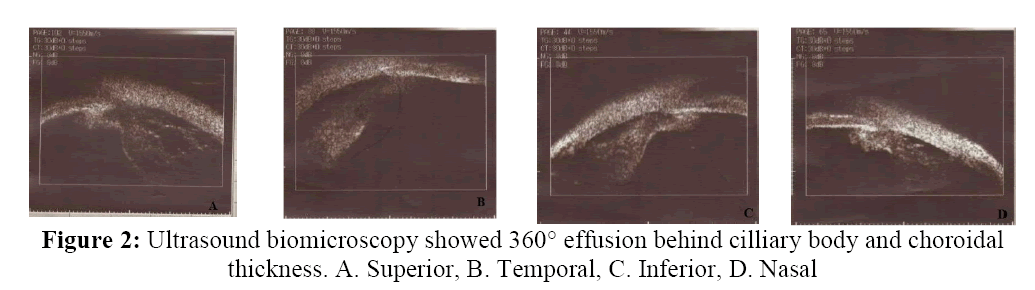
About one month after ALPI, he was referred to his ophthalmologist with blurred vision of right eye from three days ago; visual acuity of right eye was 0.3 and not corrected. The right anterior chamber was markedly shallowed and the IOP was 21 mmHg. There were no signs of inflammation. Indirect ophthalmoscopy revealed a multilobular choroidal detachment (figure 1). Ultrasound biomicroscopy revealed 360° effusion behind cilliary body and choroidal thickness (figure 2).
Tablet of prednisolone 50 mg was started for patient and tapered for two months. Choroidal effusion was response dramatically to our treatment and resolved. After six months, best corrected visual acuity was 5/10 (aided) and 6/10 (aided) for right and left eye, respectively. His IOP was 20 mmHg and 13 mmHg for right and left eye, respectively.
Discussion
This is the first report of choroidal effusion occurring subsequent to ALPI. Interestingly; the left eye did not undergo any complications treated with ALPI, even though the treatment was of similar. Choroidal effusion was started at one month after ALPI. Choroidal effusion are usually reported following intraocular surgery; Where postoperative and/or intraoperative hypotony is combined with postoperative inflammation [1]. In our case, choroidal effusion was occurred in high IOP and no evidence of inflammation. It is interesting that reabsorption of high rate of choroidal effusion occurred with medication and there was no need for surgical drainage procedures. Complications after ALPI included: Mild iritis, Hemorrhage, Pigmented burn marks, Iris atrophy, and relative prolonged mydriasis after ALPI that not respond to pilocarpine treatment [2].
Conclusion
Based on this case report, choroidal effusion appears to be another complication of ALPI; although further studies are needed to confirm this association. In the reported case, this complication and its effects were temporary and resolved with conservative management.
References
Open Access Journals
- Aquaculture & Veterinary Science
- Chemistry & Chemical Sciences
- Clinical Sciences
- Engineering
- General Science
- Genetics & Molecular Biology
- Health Care & Nursing
- Immunology & Microbiology
- Materials Science
- Mathematics & Physics
- Medical Sciences
- Neurology & Psychiatry
- Oncology & Cancer Science
- Pharmaceutical Sciences