Predictors of Breast Cancer Survival in a Tertiary Care Hospital in Coastal Karnataka
Nair Suma, Atreya R Mihir, Kathrikolly Thejas, Kamath Asha, Mamidipudi S Vidyasagar
Nair Suma (MD)*, Atreya R Mihir (MBBS), Kathrikolly Thejas (Msc), Kamath Asha (PhD), Mamidipudi S Vidyasagar (MD)
Kasturba Medical College, Manipal University, Manipal
- *Corresponding Author:
- Nair Suma
Department of Community Medicine Kasturba Medical College, Manipal University,
Manipal Karnataka – 576104, India
Tel: +91- 820 – 2922723 (O)
Email: suma.nair@manipal.edu, sumavimal@gmail.com
Abstract
Background and Objectives: Breast cancer survival is sparingly addressed in India due to inadequate follow-up, lack of organized screening activities and an incomplete system of death registration. This study analyses the specific factors affecting breast cancer survival in a tertiary care hospital. Methods: This was a five year retrospective analysis of a cohort of breast cancer patients who attended a tertiary care hospital in Southern India. Case records of 112 women fulfilling the inclusion criteria were reviewed. SES (socioeconomic status), age at menarche, family history of breast cancer, disease staging by TNM (Tumour Node Metastasis) criteria and treatment modality were some of the variables considered for estimating the hazard ratio using the Cox regression analysis. Survival probability was analysed using the Kaplan-Meier and forward Wald cox regression. Results: Women in the study were predominantly (68%) from the lower socio economic strata with more than half (57%) being less than 50 years of age. Seventy two percent of them presented with a local extension of the disease while 13% had evidence of distant metastasis. Overall mean survival rate was noted to be 53.7 months (95% CI 51.6, 55.9). Stage at diagnosis (distant metastasis) (RR 5.11, 95% CI 1.599 – 16.334, p < 0.05) and age at menarche (< 14years) (RR 2.866, 95% CI (1.175 – 6.990), p < 0.05) were found to have a significant impact on the outcome. The reported death rate among the study population was 27.7%. Conclusion: This study shows a promising overall 5 year disease survival where stage at diagnosis was found to be an important predictor. Increasing awareness about early detection coupled with an organised screening programme that coordinates with existing treatment facilities could go a long way in improving the mortality burden due to breast cancer in the country.
Keywords
Breast cancer, survival rates, stage at diagnosis
Introduction
Breast cancer incidence rates have been increasing and this increase is most noticeable in previously low prevalence areas such as the Asian continent [1]. Statistics from India concur on this as breast cancer is noted to be the leading cancer in metros like Mumbai and Bangalore [2]. This rising trend has been attributed to changing life styles owing to rapid industrialization and urbanization in a fast growing economy [3] and scant screening activities [1].
In comparison to developed countries, survival among breast cancer patients is sparingly addressed in India. This is primarily due to inadequate follow-up, lack of organized screening programs and an incomplete system of registration of deaths which are vital for estimating survival rates. All the same, existing data show an encouraging trend from an overall five year survival rate of 40% in the early 90s [4] to nearly 77% in 2008 [5]. This favourable statistic is a reflection of the advances in the field of breast cancer treatment as curability is an important predictor of survival. However, in countries like India curability is indirectly determined by sociocultural dynamics, lack of awareness and inadequate resources for treatment [6]. In this context we estimated the survival among breast cancer patients over a five year period and explored the association of demographic and reproductive factors as well as stage of disease at presentation.
Methods
Our study reviewed a cohort of breast cancer patients who had registered at a tertiary care centre in coastal Karnataka in Southern India. The setting was a teaching hospital with a dedicated cancer facility and a well-developed Health Information System. The five year retrospective analysis included data for patients registered in a particular year (ranging from 2003 to 2005) with a diagnosis of primary breast cancer. We targeted the earlier years, as we had initiated a breast health awareness initiative in the community from the year 2001. This we believed would have enhanced the treatment seeking behaviour among the local population. Data was excluded if the documentation was incomplete, patient had not completed the initial treatment or if the tumour was not graded as per the TNM criteria. Accordingly, a total of 112 records were eligible for analysis from nearly 600 registered cases. Relevant information over a 5 year period was extracted using a data extraction sheet.
Statistical Methods
A descriptive analysis was used to characterise the study population and the stages of breast cancer. Variables that were considered for estimating the hazard ratio using the Cox regression analysis were: age at diagnosis (less than 50 years was the reference variable compared to >50 years), SES (high SES was considered the reference variable in comparison to low SES), age at menarche (<14 years versus >14 years), family history of breast cancer, disease staging according to the TNM criteria and treatment modality. Survival probability was analysed using the Kaplan-Meier product limit method and multivariate analysis was done using forward Wald cox regression. Statistical analysis was done using SPSS version 15; evidence of significance was considered at p < 0.05.
Ethical clearance was obtained from the Institutional Ethics Committee. Due consent and permission was obtained to access the medical records of the patients, which were coded to ensure confidentiality.
Results
Table 1 depicts the characteristics of the study population which shows majority (67.8%) to be from the lower socio economic strata and composing primarily of women less than 50 years of age (mean age 47.8 +10.5 years). Kuppuswamy’s SES scale [7] was used to categorise socioeconomic status of the women. More than half the women were from the district where the facility was located, while the remaining were referred from other parts of the state. Almost 99 % of the women had attained menarche after 11 years of age and nearly 93 % of them had no history of breast cancer among first degree relatives. The median follow up time in the present study was 60 months and the reported overall death rate among the study population was 27.7%.
| FACTORS | NUMBER (PERCENTAGE) |
|---|---|
| Age at diagnosis | |
| ≤ 50 Years > 50 Years |
64 (57.1) 48 (42.9) |
| Place of residence | |
| Within the coastal district Outside the coastal district |
57 (50.9) 55 (49.1) |
| Socio Economic Status | |
| High and Middle Low |
36 (32.2) 76 (67.8) |
| Age at menarche | |
| ≤ 14 Years > 14 Years |
70 (62.5) 42 (37.5) |
| Menstrual status | |
| Pre menopause Post menopause |
55 (49.1) 57 (50.9) |
| Number of children | |
| No children 1 or more child |
05 (04.5) 107 (95.5) |
| Family history of breast cancer | |
| Yes No |
08 (07.1) 104 (92.9) |
Table 1: Characteristics of the study population
While the tumour grade could not be assessed in a quarter of the study population, a significant majority (72%) showed local extension of the disease and more than half (56.3%) presented with regional spread to the lymph nodes. Thirteen percent of the patients had evidence of distant metastasis at the time of diagnosis. Fourteen percent of women hailing from local areas presented with distant metastasis, which was similar to that found among women hailing from neighbouring states. Most utilised mode of treatment was surgery (92.1%), followed by chemotherapy (79.5%), radiotherapy (75.9%) and hormonal therapy (46.4%). While selfdiscovery was the primary mode of detection in 65% of the women, the other 35% had subjected themselves to an annual clinical breast examination.
Death as an outcome was the event studied. Table 2 shows the analysis of 5 year survival rates with respect to the prognostic factors considered. Demographic factors like age at diagnosis and socioeconomic status did not show a significant association. Likewise the number of children borne by the woman or menstrual status did not show any significant influence on the outcome. Interestingly women with a family history of breast cancer had a non- significant better prognosis than women without any family history. Survival rates of women who had attained menarche at 14 years or earlier were noted to be significantly poor. Disease related factors like distant metastasis at the time of diagnosis (RR 5.11, 95% CI 1.599 – 16.334, p < 0.05) and having had no surgery (RR 9.195, 95% CI (3.853 – 21.945, p < 0.05) were noted to be significantly associated with poor survival.
| VARIABLE | RR (95% CI) | ADJUSTED RR (95% CI) |
|---|---|---|
| Age at diagnosis | 1.300 (0.643 – 2.629) | |
| SES | 1.016 (0.479 – 2.158) | |
| Age at menarche | 2.866 (1.175 – 6.990) * | 2.816 (1.132 – 7.004) * |
| Family history of breast cancer | 0.395 (0.054 – 2.893) | |
| Number of children | 2.324 (0.705 – 7.666) | |
| Menstrual status | 1.067 (0.527 – 2.158) | |
| Stage at diagnosis | 5.111 (1.599 – 16.334) * | 4.890 (1.529 – 15.637) * |
| Type of treatment | 0.728 (0.312 – 1.697) | |
| Having had no surgery | 9.195 (3.853 – 21.945) * |
Table 2: Relative Risk (RR) of breast cancer death in univariate and multivariate analysis
Multivariate analysis adjusting for other prognostic factors showed stage at diagnosis (distant metastasis) and age at menarche (< 14years) (RR 2.866, 95% CI (1.175 – 6.990), p < 0.05) to have a significant impact on the outcome.
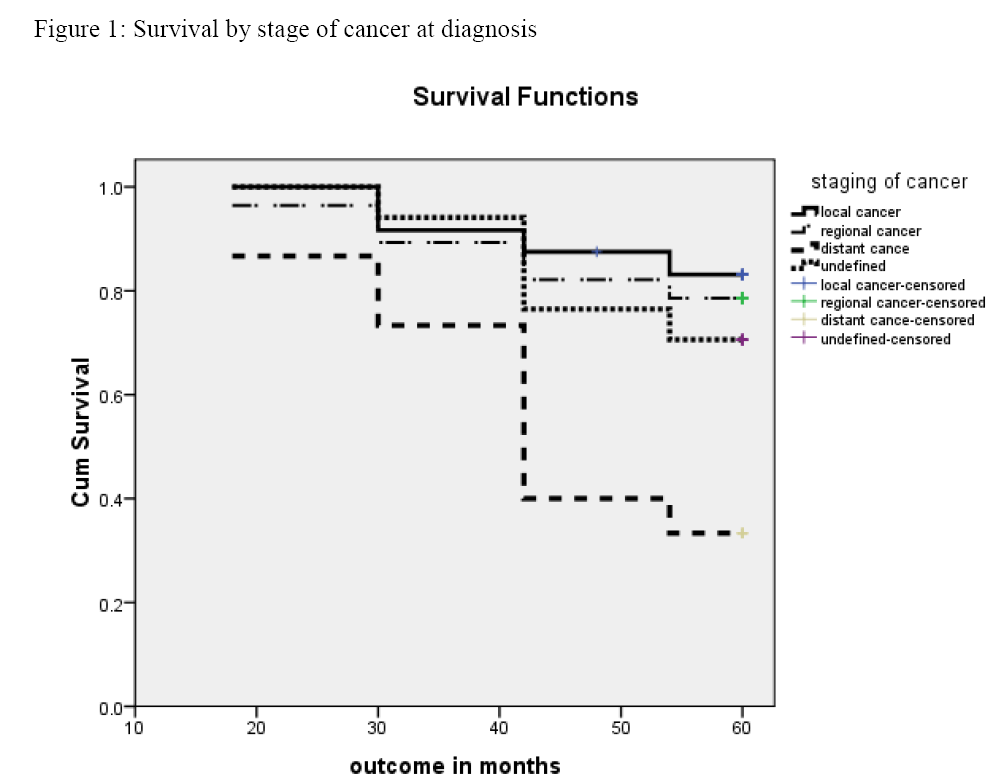
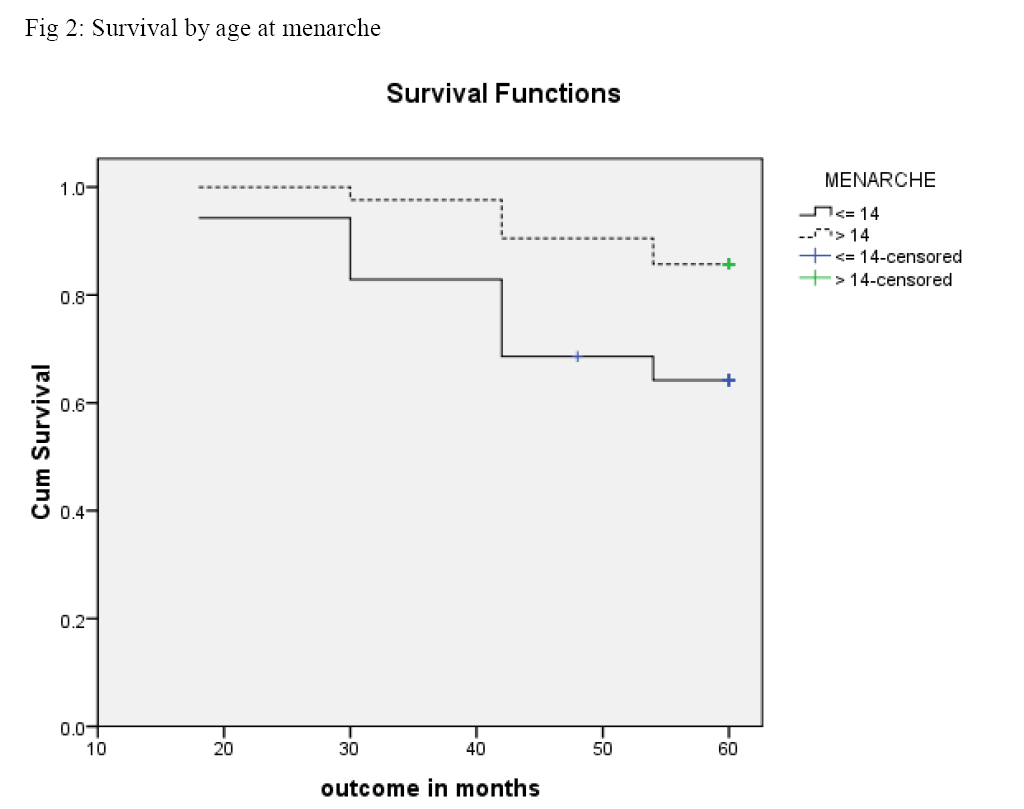
Overall mean survival rate was 53.7 months (95% CI 51.6, 55.9). The five year survival rate of patients with local and regional cancer showed an encouraging 88% and 81% respectively (Fig.1). Conversely, only 33% of those with distant metastasis and 64% of those who had an earlier menarche (Fig. 2) survived for a period of 5 years.
Discussion
Estimation of survival rates is important as it gives an insight into the various prognostic factors of a disease. Here we have looked at the survival for a total period of 60 months. Lack of access to a centralized registration system unlike in the west, made this a daunting task and probably the reason why there are few studies addressing this issue in India. In comparison to other studies reported from India, [4,5,8,9] this study differed with respect to certain predictors; age at diagnosis and menarche being the two notable ones. In addition a better overall survival rate was also observed in comparison to existing literature from India.
Age at diagnosis has been shown to be an important predictor of survival in many settings. Ganesh et al [5] in their study, found that younger patients (< 50 years) had a better survival rate of 81% when compared to older patients (>50 years). Similar findings have also been reported by Sant et al [10] from Italy as well as Gajalakshmi et al [8] from Chennai, India. Our study however, did not support these findings and concurred more with Barchielli et al, [11] who stated that age at diagnosis was not significantly associated with breast cancer survival and that worse prognosis in the elderly was probably due to the risk of death from other causes, rather than a different malignant potential of the tumour. This observation could be further explored with more robust studies in future.
Orgeas et al [12] demonstrated a significant impact of age at menarche (11 years or earlier) on breast cancer prognosis and survival among Swedish women. As majority of the women in our study had attained menarche after 11 years of age we were unable to study this association. Our study however, demonstrated an association with 14 years or earlier age at menarche. Nair et al [4] in their study set in Kerala and Alsaker et al [13] from Norway did not find an association with this variable. This finding raises the question whether a uniform cut off value could be used to define early menarche across populations. This is another area that requires further investigation.
Stage of breast cancer at diagnosis is an important predictor of breast cancer survival. This is evident in this study as patients presenting with distant metastasis had a poor overall survival rate of 33 % as compared to those with local extension (88%). This finding is in concurrence with several studies [4,5,8,9]. Gajalakshmi et al [8] in their study reported overall survival rates for localised disease, regional disease and distant metastasis as 63.6%, 52.4% and 25.5% respectively. Our study showed better rates in all three categories and the findings corroborate western statistics [14] wherein the reported survival rates are 98%, 84% and 23% respectively for each of the three defined stages. This improvement in survival could be attributed to the progression in understanding the disease and better treatment guidelines since the beginning of the new millennium. Besides, internet accessibility has improved communication like never before thus enabling sharing of these evidences with people at large.
However, it must be stated that there was no difference in the proportion of cases presenting with distant metastasis with respect to the region they hailed from. Local women were as likely to present with distant metastasis as women from other parts of the state or outside the state. This probably stresses the need to further enhance the reach of the breast health initiative introduced by us.
As seen elsewhere, [15] these women also reported self –detection as a common mode of recognising a breast abnormality. This reaffirms the importance of breast self -examination as a screening mechanism especially in low resource settings, where other screening modalities may be inaccessible.
Meng et al, [16] Pollock et al [17] and Thomson et al [18] in their respective studies had showed an association between low socio-economic status and poor overall survival rates. We failed to appreciate this association as nearly 68% of the population were from the low SES.
Our study revealed a significantly better survival among the group that underwent surgery in comparison to those who did not. This was however not illustrated in the multivariate analysis. This is because treatment depends on the clinical stage at presentation and therefore cannot be considered an independent prognostic factor. Ganesh et al [5] in their study have illustrated a similar finding.
There are certain inherent limitations in this study. This being a hospital based retrospective data, selection bias is a possibility. However, as this is the only dedicated cancer treatment facility in the area, community pattern maybe reflected to an extent. The effect of some important variables such as mode of self- detection (either by BSE or accidental) and specific treatment modality was difficult to assess with the retrospective design.
Conclusion
This study shows an encouraging overall 5 year survival from breast cancer and endorses stage at diagnosis to be an important predictor. Considering that self – discovery was the common mode of detection among this population, training and educating women about breast self - examination could enhance breast health awareness [19] thereby serving as an important screening intervention for early detection. In addition there is an urgent need to identify how heightened awareness about the disease coupled with better self- examination skills could be coordinated with existing treatment facilities. This could be further strengthened by pragmatic, cost effective public health research in the area.
List of abbreviations
1. SES – Socio-economic status
2. BSE – Breast self - examination
3. TNM – Tumour Node Metastasis
IRB Permission: Obtained from Kasturba Hospital ethics committee bearing the reference number IEC-024/009
Grant Registration Number: 21/KA/KMCMP-70/09-BMS
Competing Interests: Nil
Authors‘ Contributions
| Contributor 1 | Contributor 2 | Contributor 3 | Contributor 4 | Contributor 5 | |
| Concepts | ÃÆâÃâà âÃâââ¬Â | ÃÆâÃâà âÃâââ¬Â | ÃÆâÃâà âÃâââ¬Â | ||
| Design | ÃÆâÃâà âÃâââ¬Â | ||||
| Definition of intellectual content |
ÃÆâÃâà âÃâââ¬Â | ÃÆâÃâà âÃâââ¬Â | ÃÆâÃâà âÃâââ¬Â | ÃÆâÃâà âÃâââ¬Â | ÃÆâÃâà âÃâââ¬Â |
| Literature search | ÃÆâÃâà âÃâââ¬Â | ÃÆâÃâà âÃâââ¬Â | ÃÆâÃâà âÃâââ¬Â | ||
| Clinical studies | |||||
| Experimental studies | |||||
| Data acquisition | ÃÆâÃâà âÃâââ¬Â | ||||
| Data analysis | ÃÆâÃâà âÃâââ¬Â | ÃÆâÃâà âÃâââ¬Â | |||
| Statistical analysis | ÃÆâÃâà âÃâââ¬Â | ÃÆâÃâà âÃâââ¬Â | |||
| Manuscript preparation | ÃÆâÃâà âÃâââ¬Â | ÃÆâÃâà âÃâââ¬Â | ÃÆâÃâà âÃâââ¬Â | ||
| Manuscript editing | ÃÆâÃâà âÃâââ¬Â | ÃÆâÃâà âÃâââ¬Â | |||
| Manuscript review | ÃÆâÃâà âÃâââ¬Â | ÃÆâÃâà âÃâââ¬Â | ÃÆâÃâà âÃâââ¬Â | ÃÆâÃâà âÃâââ¬Â | |
| Guarantor | ÃÆâÃâà âÃâââ¬Â |
Acknowledgement
We acknowledge Indian Council of Medical Research for the short term student research support to Mihir Atreya as well as Kasturba Medical College, Manipal and Manipal University for internal support.
References
- Global Cancer Facts & Figures. 2nd ed.; 2011. Available at:https://www.cancer.org/acs/groups/content/@epidemiologysurveilance/documents/document/acsp c-027766.pdf. Accessed August 12, 2015.
- NCDIR-NCRP, Bangalore, India. Consolidated Report of Hospital Based Cancer Registries: 2007-2011.; 2011:95-100. Available at:https://www.ncrpindia.org/ALL_NCRP_REPORTS/HBCR_REPORT_2007_2011/ALL_CONTE NT/PDF_Printed_Version/Chapter10_Printed.pdf. Accessed June 18, 2014.
- Murthy NS, Chaudhry K, Nadayil D, Agarwal UK, Saxena S. Changing trends in incidence of breast cancer: Indian scenario. Indian J Cancer. 2009; 46: 73-74
- Nair MK, Sankaranarayanan R, Nair KS, Amma NS, Varghese C, Padmakumari G, et al. Overall Survival from breast cancer in Kerala, India, in relation to menstrual, reproductive and clinical factors. Cancer. 1993; 71: 1791-1796
- Ganesh B, Talole SD, Dikshit R, Badwe RA, Dinshaw KA. Estimation of survival rates of breast cancer patients - a hospital- based study from Mumbai. Asian Pac J Cancer Prev. 2008; 9: 53-57
- Hanna TP, Kangolle AC. Cancer control in developing countries: using health data and health services research to measure and improve access, quality and efficiency. BMC Int Health Hum Rights. 2010; 10: 24.
- Sharma R. Kuppuswamy's socioeconomic status scale - revision for 2011 and formula for real-time updating. Indian J Pediatr. 2012; 79(7): 961-962.
- Gajalakshmi CK, Shanta V, Swaminathan R, Sankaranarayanan R, Black RJ. A population-based survival study on female breast cancer in Madras, India. Br J Cancer. 1997; 5: 771-775
- Babu GR, Lakshmi SB, Thiyagarajan JA. Epidemiological Correlates of Breast Cancer in South India. Asian Pac J Cancer Prev. 2013; 14: 5077-5083
- Sant M, Gatta G, Micheli A, Verdecchia A, Capocaccia R, Crosignani P, et al. Survival and age at diagnosis of breast cancer in a population-based cancer registry. Eur J Cancer. 1991; 981-984
- Barchielli A, Balzi D. Age at diagnosis, extent of disease and breast cancer survival: a population-based study in Florence, Italy. Tumori. 2000; 86: 119-123.
- Orgéas CC, Hall P, Rosenberg LU, Czene K. The influence of menstrual risk factors on tumor characteristics and survival in postmenopausal breast cancer. Breast Cancer Res. 2008; 10: R107
- Alsaker MD, Opdahl S, Asvold BO, Romundstad PR, Vatten LJ. The association of reproductive factors and breastfeeding with long term survival from breast cancer. Breast Cancer Res Treat .2011; 130: 175-182.
- American Cancer Society. Breast Cancer Facts & Figures 2011-2012. Atlanta: American Cancer Society, Inc;2011
- Mara YR, Joann GE, Joyce PY, Lisa MR, Natalia VO, Diana LM. Self-Detection Remains a Key Method of Breast Cancer Detection for U.S. Women. J Womens Health (Larchmt). 2011; 20(8): 1135–1139. doi:10.1089/jwh.2010.2493
- Meng L, Maskarinec G, Wilkens L. Ethnic differences and factors related to breast cancer survival in Hawaii. Int J Epidemiol. 1997; 26: 1151–1158
- Pollock AM, Vickers N. Breast, lung and colorectal cancer incidence and survival in South Thames Region, 1987–1992: the effect of social deprivation. J Public Health Med. 1997; 19: 288–294
- Thomson CS, Hole DJ, Twelves CJ, Brewster DH, Black RJ; Scottish Cancer Therapy Network. Prognostic factors in women with breast cancer: distribution by socioeconomic status and effect on differences in survival. J Epidemiol Community Health. 2001; 55: 308–315
- Rao RS, Nair S, Nair NS, Kamath VG. Acceptability and effectiveness of a breast health awareness programme for rural women in India. Indian J Med Sci. 2005; 59: 398-402
Open Access Journals
- Aquaculture & Veterinary Science
- Chemistry & Chemical Sciences
- Clinical Sciences
- Engineering
- General Science
- Genetics & Molecular Biology
- Health Care & Nursing
- Immunology & Microbiology
- Materials Science
- Mathematics & Physics
- Medical Sciences
- Neurology & Psychiatry
- Oncology & Cancer Science
- Pharmaceutical Sciences