Cardio-Oncology Programs in the United States
Okwuosa TM, Yakupovich A
| Okwuosa TM*, Yakupovich A Assistant Professor, Department of Internal Medicine, Division of Cardiology, Rush University Medical Center, Chicago, USA |
| Corresponding Author: Okwuosa TM, Assistant Professor, Department of Internal Medicine, Division of Cardiology, Rush University Medical Center, Chicago, USA, Tel: 3129424601; Email: tokwuosa@rush.edu |
Abstract
As cancer patients live longer, many of them are dying from heart disease as a result of the intense oncologic treatment which they received prior. Cardio-oncology has gained significant momentum as a subspecialty able to bridge the field of cardiology and oncology, ensuring that oncology patients with heart disease receive necessary lifesaving oncology therapy, while their heart disease is being managed in order to prevent cardiovascular sequelae. Nonetheless, establishing a cardio-oncology program has its challenges, including decisions on clinic location, roles of clinic staff, in-patient consultation services, lack of mentorship, lack of guidelines for clinical practice, and so on. This paper hopes to address some of these issues by providing physicians interested in pursuing a career in cardio-oncology, as well as administrators interested in creating a cardio-oncology program, an outline of what to expect when attempting to build a successful practice.
Keywords |
||||
| Cardio-Oncology, Onco-Cardiology, Cancer, Patient, Cardiology, Clinic Program, Epidemiology, Chemotherapy, Radiation therapy | ||||
Introduction to Cardio-Oncology |
||||
| Cardiovascular disease and cancer have been the leading causes of death for nearly a century and in 2010 they accounted for 46% of all deaths in the United States [1]. Nonetheless, there has been much success in finding treatments and cures for these patients. According to the American Cancer Society there will be an estimated 19 million cancer survivors in the U.S. by 2024 with an overall survival rate of 66% [2]. Improvements in cancer therapies mean that increasing numbers of patients live many years after successful treatment. In the past, the leading cause of death was cancer recurrences, but nowadays deaths are frequently attributed to premature cardiovascular disease [3]. A prospective cross sectional study of 1853 adult survivors of childhood cancer were found to have an increased prevalence of cardiac conditions ranging from 3-24% in survivors aged 30-39 and 10-37% in those aged 40 or older [3]. Specifically these survivors had a 7.4% incidence of cardiomyopathy, 3.8% of coronary artery disease, 4.4% of rhythm abnormalities and 28% incidence of valvular regurgitation or stenosis [3]. Thus, in an effort to manage patient health as they traverse through their cancer therapy a clinical discipline termed “cardio-oncology” has evolved. Cardiooncology aka “onco-cardiology” focuses on preventing and/or treating cardiac disease as best as possible alongside a patient’s cancer therapy. | ||||
Role and Challenges of Onco-Cardiologists |
||||
| With the advent of radiation therapy and anthracyclines in the 1900s and 1950s respectively, clinicians were alerted to the cardiotoxic effects of cancer therapy (Table 1). Furthermore, the development of new cancer therapeutic agents has greatly evolved in recent years and so too has the varying degree of cardiovascular toxicities associated with them. In addition, cancer treatment often introduces patients to unfavorable conditions such as low platelet counts, hypercoagulability, dehydration and deconditioning. This presents a real challenge to the oncologist, who might be reluctant to give life-saving cardiotoxic therapy due to potentially aggravating cardiovascular comorbidities. Consequently, there arose a need for cardiologists to acquire the skills and understanding necessary to prevent, diagnose and manage these conditions, thus necessitating the field of cardio-oncology. Similar to specialties such as cardiorenal and cardiogeriatrics which have identified a need to merge specialties and outlined models for clinics and programs to follow [4,5], cardio-oncologists or onco-cardiologists, occupy a role that bridges the two specialties in order to better manage the foremost causes of death in the U.S. and the world in general. | ||||
| Recently the American College of Cardiology (ACC) recognized cardio-oncology as a sub-specialty society under its umbrella. However, onco-cardiologists still face many challenges including the acquisition of resources such as mentorship, research funding, clinical staff training, administrative assistance, establishing a consultation service and most importantly finding a location to build their practice. | ||||
Choice of Practice Location |
||||
| An effective cardio-oncology practice would require prompt delivery of patient care with the ability to coordinate with oncologists, as well as rapid access to cardiological testing, particularly ECG and echocardiography. | ||||
| A cardio-oncology clinic in a cancer center has the capacity to offer more inclusive care of the cancer patient. In such a situation, the cancer center not only facilitates infusions and other cancer related services but could provide the added benefit of a cardiovascular service in the same location. This is a particularly important point since cancer patients are commonly quite ill and weak, making it more difficult to maintain their numerous outpatient appointments, particularly in different locations. Conversely, the use of an institutional cancer center may still pose the problem of access to cardiovascular studies such as ECG, echocardiography, stress tests, etc. Securing at least an ECG machine is necessary at the site to possibly provide initial evidence of cardiac abnormalities; and procurement of an echocardiography machine would make for more efficient establishment of a cardiovascular diagnosis. However, these machines are not always deemed necessary in the institutional budget. | ||||
| Establishing a cardio-oncology clinical service within a cardiology clinic has some merit, and also produces some disadvantages. A cardiology clinic has the advantage of a support staff that is familiar with the spectrum of cardiovascular disease, in addition to patient and provider proximity to cardiovascular services such as an ECG and Echocardiogram. However, the drawback of this paradigm include the lack of awareness by the oncologist of the special cardiology services dedicated to oncology patients leading to less spontaneous consultations and interactions between the two providers. Furthermore, this approach would require cardiology clinic staff to further train on chemotherapy and radiation treatment, as well as patient needs, to ensure that proper frequent monitoring and follow up is maintained. | ||||
Training the Clinical Staff |
||||
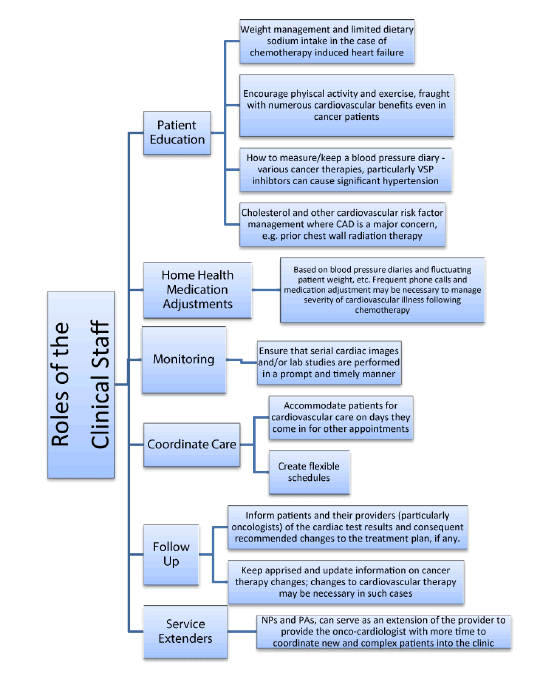
| Clinical staff such as medical assistants, nurses, and physician extenders (NPs/PAs) acts as the face of the cardio-oncology program. They are a crucial in managing the complexity of illness of the cardio-oncology patient, just by the fact that it encompasses two vastly different medical specialties. Consequently, the staff help serve as a bridge between the 2 specialties (Figure 1). | ||||
| One of the major challenges in establishing a comprehensive cardio-oncology service in an oncology center is that of finding clinical staff and mid-level providers with an interest or training in both fields of internal medicine (cardiology and oncology). In a cancer center, such a clinic would require staff training in performing ECGs, answering questions and educating patients on blood pressures, cholesterol, post cardiac catheterization management, etc. If located within a cardiology clinic the support staff would be able to manage these cardiovascular services at the expense of losing the oncological training and understanding of the special needs some cancer patients may require. However, both groups of clinical staff would require additional training on understanding the cardiovascular abnormities that might be prevalent with certain chemotherapies, so that more frequent monitoring and follow up may established. | ||||
Inpatient Consultation Services |
||||
| For expanded services, some cardio-oncology programs may have a dedicated in-patient consultative service. The benefit of this program would be the rapid and frequent involvement of onco-cardiologists with patients undergoing cancer therapy; and in some cases, could provide prudent or even potentially lifesaving therapy in patients whose lives lie between the balance beams of cardiovascular disease and cancer. | ||||
| Such expanded service would likely require two or more practicing onco-cardiologists as well as support staff within an institution. As such, the frequency of consultations would depend mostly on the size and consultation culture of the institution, in addition to the oncology services offered (cardiology consultative services are more frequently required in programs that offer stem cell transplantation and engage in frequent clinical trials). However, two onco-cardiologists are not always a requirement. An institution with only one practicing onco-cardiologist and limited support staff could adopt an approach where the general cardiology service sees and consults on the cancer in patient with/without some input from the onco-cardiologist, with subsequent cardio-oncology outpatient follow-up. | ||||
Administrative Roles |
||||
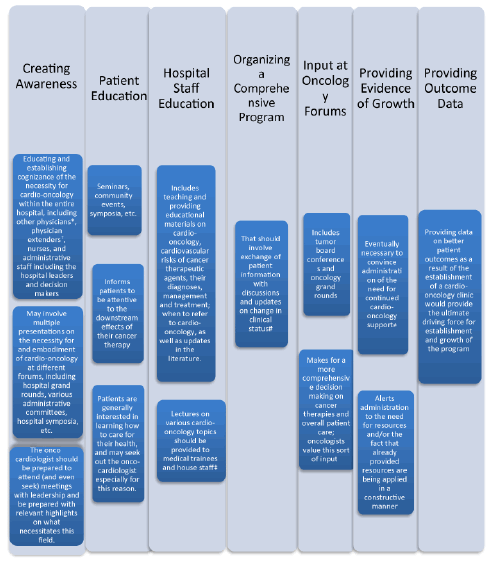
| As a new field in cardiology, a crucial element to the success of any cardio-oncology program is that the institutional administration views the program as a bourgeoning field, and as an essential component of any comprehensive cardiology program. The patient make-up of a cardio-oncology clinic include those who present for pre-cancer therapy evaluation, those currently undergoing cancer therapy, or cancer survivors status post cancer therapy which have cardiovascular side effects that could span up to 20-30 years. A well-informed administration understands the wide-ranging patient composition and could provide the necessary support to encourage the growth of the program. This is extremely important because institutional administrative support is usually tied to the size of the linked oncology program referral base, and certain administrative approaches could facilitate greater institutional assistance (Figure 2). | ||||
| An institutional administration supports and dedicates time to a growing cardio-oncology program. Necessary support includes: | ||||
| a] Providing support staff. | ||||
| b] Enabling the onco-cardiologist to engage and develop the program by attending various oncology tumor board conferences, particularly those involving chest wall radiation and/or employing chemotherapeutic options that are known to be cardiotoxic. | ||||
| c] Creating time for educating other staff and programs within the institution, e.g. giving conferences specifically to tumor boards on different aspects of cardio-oncology, including imaging and predictive factors for cardiotoxicity. | ||||
| d] Afford time and resources to establish a cardio-oncology database. This could be pivotal in ensuring easy access to data for both research and cardio-oncology clinic progress. This should involve both oncology and cardiology variables, and would help establish the name of the institution in the field of cardio-oncology. | ||||
Research/Mentoring in Cardio-Oncology |
||||
| Research is paramount in the recognition of an institution as an expert in any field including that of cardio-oncology. Being a nascent field, there is yet limited data and much yet to be understood regarding the relationship between cancer, cancer therapy and the heart. This leaves a lot of questions unanswered, which makes cardio-oncology a field wide open for research. | ||||
| Nonetheless, funding in unknown fields can be challenging, as funding agencies are less apt to sponsor a project that is less understood. To address these research needs, a number of workshops and consensus statements have convened and published material recognizing gaps in cardio-oncology research, as well as the growing need for researching advances in the field, particularly those that could be applied to large population groups [6-9]. | ||||
| Because cardio-oncology is a particularly new field made up of young faculty in the process of establishing their own program, finding a mentor/senior faculty who could engage in cardio oncology research in one’s own institution could be difficult. Oftentimes an onco-cardiologist must secure a mentor in one of the few major cancer centers in the country such as MD Anderson, Sloan Kettering Cancer Center or Dana- Farber Cancer Institute. However, it should be noted that although having a faculty mentor in an already established cardio-oncology program may be beneficial, the long distance mentor-mentee relationship may generate less opportunities for contact and therefore lead to less motivation and less accomplished work in this fascinating field. | ||||
Conclusion |
||||
| Cardio-oncology is a rising sub specialty dealing with cardiovascular diseases in cancer patients, either as a result of cancer therapy or cancer itself. This unique specialty establishes the onco-cardiologist – usually a cardiologist – as an important player in the field of oncology. Nonetheless, building a cardio-oncology program has its challenges including but not limited to hospital/institutional administration in obtaining resources, training of clinical staff, and establishing the proper location for the cardio-oncology clinic. Although this presents a difficult road for an onco-cardiologist, the challenges could be overcome with someone who is extremely interested, driven, judicious with time and resource management, and a great team player who is able to merge two different medical specialties for more comprehensive patient care. | ||||
Tables at a glance |
||||
|
||||
Figures at a glance |
||||
|