Work Related Musculoskeletal Disorders in Female Nursing Personnel: Prevalence and Impact
Nur Azma BA, Rusli BN, RM Noah, Oxley, JA, Quek KF
Nur Azma BA1,2*, Rusli BN1, RM Noah2, Oxley, JA3, Quek KF1
1Jeffrey Cheah School of Medicine and Health Sciences, Monash University Malaysia Jalan Lagoon Selatan, Bandar Sunway, 46150 Selangor Darul Ehsan, Malaysia
2Universiti Kuala Lumpur, Institute of Medical Science Technology Jalan TKS 1, Taman Kajang Sentral, 43600 Kajang, Selangor, Malaysia
3Monash Injury Research Institute Building 70, Monash University, Victoria 3800, Australia
- *Corresponding Author:
- Nur Azma Amin
Jeffrey Cheah School of Medicine and Health Sciences
Monash University Malaysia Jalan Lagoon Selatan, Bandar Sunway
46150 Selangor Darul Ehsan, Malaysia
Email: naami5@student.monash.edu, wnm7912@gmail.com
Abstract
Introduction: There is substantial evidence showing that work related musculoskeletal disorders (WRMSDs) have become a common occupational health problem in nursing population. Objectives: This study aims to investigate the prevalence and impact of WRMSDs among nurses in public hospitals in the Klang Valley. The study also evaluated the reliability of the Malay version of the Standardized Nordic Musculoskeletal Questionnaire (M-SNMQ). Methods: A cross-sectional study was conducted among 660 female nurses working in four selected public hospitals in the Klang Valley, Malaysia. The validated M-SNMQ was used to estimate the prevalence and impact of WRMSDs. The socio-demographic and occupational information were also obtained from the nurses. Results: A total of 77.4% response rate was achieved with 376 nurses completing the survey. Of these, 88.6% (n=333) and 73.1% (n=275) experienced symptoms of WRMSDs in their lifetime and for the past 12 month respectively. Neck (48.9%) was the most prevalent site followed by feet (47.2%), upper back (40.7%) and shoulders (36.9%) and of those, the majority sustained at least moderate pain. Less than 25% of the nurses agreed that WRMSDs affected their quality of life. The result if Kappa agreement indicates a good level of test –retest reliability of M-SNMQ. Hence, proven that the M-SNMQ is a reliable instrument to assess the presence of WRMSDs among female nurses in Malaysia. Conclusions: These findings suggests that WRMSDs is relatively high among the studied Malaysian nurses. Further study should be undertaken to identify the potential risk factors to reduce the prevalence in the near future.
Keywords
Work related musculoskeletal disorders, nurses, reliability, Nordic musculoskeletal questionnaire
Introduction
Over decades, a number of researchers reported high rates of workplace injury within the health care industry [1,2] including work related musculoskeletal disorders (WRMSDs) [3]. WRMSDs are categorized as non-communicable disease and best described as disorders or discomforts sustained by the worker on the musculoskeletal, peripheral nerves, and neurovascular systems resulting from prolonged exposure to workplace hazards. Simple movements are often difficult and painful [4]. WRMSDs were known by many terms and have been used interchangeably with Repetitive Motion Injuries (RMI), Cumulative Trauma Disorder (CTD) and Repetitive Strain Injuries (RSI).
WRMSDs accounted for 34% of workplace illnesses with an incidence rate of 38 cases per 10,000 full-time workers [5]. For decades, WRMSDs among healthcare workers, and among nursing staffs in particular, are of major concern worldwide [6–12]. A number of literatures documented high annual prevalence of WRMSDs in at least one body region that varied between 40% to 95% in Asian populations [13–17] and Western populations [18–20]. Lower back (29% - 64%) [11,21,22], neck (34%- 63%) [10,13,15,23,24], and shoulders (17% - 75%) [9,10,16,17,25–27] were among the most prominent affected areas.
The impacts of WRMSDs are not only borne by the individual [23,28], but also the employer, and society either direct or indirectly [29,30]. The direct effects included lost working time, medical bills, wages paid during absence, workers’ insurance funds, and individual’s quality of life [3]. Indirect effects represented approximately 75% of overall costing involving dependent benefits, cost of additional workers, psychological difficulties, production downtime, workers’ compensation claims, job changes and turnover [31]. These costs represented 4% of the world’s Gross Domestic Product (GDP) which includes the cost of injury, death and disease through absence from work, sickness treatment, disability and survivor benefit and are rarely considered [32]. In 2010, the total disbursement of temporary disablement was RM109 million; for permanent disability benefits, it amounted to RM306 million, and dependent benefits cost RM205 million [33]. On the other hand, research from Australia disclosed that half of 955 nursing personnel admitted taking leave due to work- related injuries or diseases with 71% of them sustaining WRMSDs [34]. Additionally, WRMSDs were also found to be a popular reason for nurses to quit their nursing professions [20,25]. As to the individuals, WRMSDs have also affected their quality of life, including functional limitations [27,28,35] and medical dependency [10,23].
In comparison to other occupational diseases, less attention was given to WRMSDs in Malaysia. In 2012, only 4% out of 1792 reported workplace accident were WRMSDs [36], which was far lower than reported in other countries. Although a number of studies discussed the prevalence of WRMSDs in Malaysia, particularly among the nursing population, none, to the authors’ best knowledge, investigated the impact of WRMSDs on the individuals affected. Thus, this study aimed to investigate the prevalence of WRMSDs and impact among Malaysian nurses. In addition, this study also assessed the reliability of the Malay-version of the Standardised Nordic Musculoskeletal Questionnaire
Material and Methods
Study design and participants
This is a cross-sectional study design involving only female nurses, aged 23-50 years old and working in shift for at least one year at the clinical sites. Exclusion criteria were: i) nurses with history of related musculoskeletal disorders prior to the study; and ii) nurses who were pregnant or at post-menopausal stage during data collection. Selection of the particular hospitals was based on convenience sampling and support from the respective hospital management. Upon receiving approval from the relevant authorities, and in collaboration with the Matron’s office at the respective hospitals, a briefing session was conducted to recruit potential participants. The study package was later distributed to those who agreed to participate in the study, through the Nurse Manager at their respective working stations. The participants remained anonymous and were identified with special identification codes which were made known only to the research team. The questionnaires were returned within a week in sealed envelopes and deposited into a locked box located at the Chief Matron’s office. Full completion of the submitted questionnaire was thoroughly checked and tokens of appreciation were given to each participant.
Sample size
The sample size was estimated using single proportion calculation [37]. Thus, to ensure an adequate sample size and power of the study, the confidence interval (CI) was set at 95%, an alpha (α) of 5% and 80% power of study. Based on the WRMSDs prevalence rate (p=78%) [38], the sample size was estimated as 264 nurses. Given an estimated 80% response, a minimum sample of 330 [(100÷80) x 264 = 330] was required. Because the nurses sampled were clustered in four public hospitals, we applied a correction factor (design effect) whereby we doubled the estimated sample size to account for this method of sampling. Hence, the questionnaires were distributed to a total of 660 (330 x 2) nurses.
In summary, 83.3% (n=550 sets) of the distributed questionnaires were returned. Of these, only 376 sets were completed and eligible for further analysis, 100 incomplete and 74 were ineligible. The eligible participants were referred to the nurses who fulfilled the inclusion criterion, whereas, ineligible were participants who were pregnant, breastfeeding mother, menopausal, and newly transferred to the current unit during the recruitment. Meanwhile, incomplete described the questionnaire with missing data of more than 20% [39]. Assuming all non-respondents were qualified for the study, the response rate was estimated at 77.4% by dividing the number of completed questionnaires (n=376) with the number of qualified nurses for the study (n=376+110=486).
In an earlier local study, according to Malaysia Ministry of Health, the Nursing of Administration nurses were graded into three categories according to the nature of work in the hospital unit, work schedule, and level of patient care [40]. Grade 1 included non-shift working nurses assigned in the out-patient clinics (such as Day care Surgery Clinics, Specialist Clinics). Group 2 consisted of shift working nurses assigned to normal in-patient wards, such as Medical and Surgical wards, Orthopaedic, Obstetrics and Gynaecology wards. Meanwhile, nursing duties in an intensive care unit included were Intensive Care Unit (ICU), High Dependency Wards (HDW), Cardiac Critical Unit (CCU), Operation theatre (OT) and Neonatal Intensive Care Unit (NICU) which are classified in Group 3. However, this study recruited only shift working nursing staffs belonging to Grade 2 and Grade 3. The authors adopted a stratified sampling approach to calculate the number of nurses from each participating hospital followed by simple random sampling.
Study material
For the convenient of the participants, the Malay translated questionnaire was used in this study. Thus for translation purposes, a multistage procedure was employed to ensure the appropriateness of the contents and equivalents between the original and translated versions, in order to reduce biasness [41]. Jones and Kay (1992) [42] suggested that at least two independent translators should be involved in the back-translation approach. Therefore, the English version of the questionnaire was initially translated into Malay language by the author and checked by the supervisors. This was followed by back-translation into English by independent bilingual translators. Both translators and authors compared the back-translated and English versions and further analysed the discrepancies including words, meanings, and contents of the respective items. The preliminary draft of the Malay translated version was pre-tested among 80 nurses working in the district hospital to identify the clarity in the translated version. The findings and comments were notified, and corrections were made accordingly. As for this study, two complementary questionnaire components formed the Malay self-administered questionnaire (SAQ). Descriptions of each questionnaire component are provided below:
Demographic and job information: This section was designed to elicit socio-demographic and job information [age, marital status, academic qualification, year of employment, hours worked per week, average monthly income and Body Mass Index (BMI)]. The Malay translated version of the Short Questionnaire of Health Enhancing Physical Activities (M-SQUASH) [43] was adopted to assess the habitual physical activities consisting of (1) commuting, (2) leisure time, (3) household activities and (4) activities at workplace. The questionnaire elucidated the frequency, intensity and duration on each involved activity across the week, respectively. Based on the Dutch Physical Guideline, activities were assigned a metabolic equivalent (MET) value, in which activities valued at ≤2 MET were discounted [44]. The distribution of intensity score according to the type of physical activity is attached in the appendix section. The choice of activities calculated for SQUASH is based on the intensity value of ≥4 MET, except for light household and light working activities. As recommended by the Ainsworth compendium, physical activities were classified into three categories: 2 to <4 MET (light), 4.0 to <6.5 MET values (moderate) and vigorous for a metabolic equivalent (MET) MET value ≥6.5. Total scores for the activity were calculated by multiplying total minutes of activity by the intensity score. Previously, minutes of activity were estimated by multiplying the frequency (days/week) and time spent (min/day). By assuming that people sleep 8 hours per day, van Berkel et al. (2013) [45] suggested that a maximum activity time involved per week shall be kept at 6720 minutes. The documented validity and test-retest reliability on SQUASH [43] has been used in research involving patients with related MSD [46].
WRMSDs symptoms were measured using the Malay translated version of Standardized Nordic Musculoskeletal Questionnaire (M-SNMQ). An anatomical diagram of nine body regions (neck, shoulder, upper and lower back, hands/wrists, arms, knee, thighs and feet) facilitated respondents to precisely identify the presence of musculoskeletal symptoms for the lifetime, preceding 12 months, past one month and last seven days [47]. Nonetheless, further investigation on the prevalence of WRMSDs was only performed for the annual prevalence because it was an appropriate time-scale similarly practiced in prior studies and was the most commonly used approach as an outcome in other epidemiological nursing studies [15,18,48]. The nurses selected ‘yes’ for the presence of any symptom (pain, numbness, tingling, aching, stiffness or burning) of WRMSDs in any anatomical site for the preceding 12 months [47]. If the participants answered ‘yes’, they were requested to answer the follow-up questions. This includes the frequency and intensity of the symptoms that occurred. The intensity was measured based on a four point Likert scale of ‘0’- “no pain” to ‘4’- severe pain. Likewise, the frequency of symptoms was assessed using the four point Likert scale of ‘0’- “never” to ‘4’- “very often”. Further, the nurses were also asked to indicate if the developing symptoms of WRMSDs in specific body sites had affected daily activities, seeking for physician, medication dependency, and/ or taking medical leave. Meanwhile, 187 nurses completed the M-SNMQ twice within approximately 3 months between the first and the second session.
Statistical analysis
The survey data was entered and analysed using IBM SPSS Statistics version 22.0 at the Jeffrey Cheah School of Medicine and Health Sciences, Monash University Malaysia. The data were reviewed for completeness and further assessed for normality distributions using the Kolmogorov-Smirnov Test. Means and standard deviations were reported for continuous parameters; frequencies and percentages were calculated for categorical data. The presence of WRMSDs was reported as prevalence rate for the preceding 12 months. The reliability of test and retest method on M-SNMQ was assessed using kappa correlation coefficient. A kappa valued greater than 0.75 indicate an excellent agreement, whilst values of a kappa between 0.40 and 0.75 are considered fair to good, and values of less than 0.40 are considered poor [49]. The phi correlation coefficient is used to estimate the association between regions, p value less than 0.05 shows significant correlations.
Results
Socio demographic and occupational profile
A majority of the nurses were Malays (94.1%), 76.4 % were married with an average age of 30.58 (SD=5.25) years. Most of them attended nursing schools and were assigned in the general or medical wards and earned an average monthly income of MYR3833.25 (SD=1536.73). More than 50% of the participants were in service for more than five years, with average service of 7.38 (SD=4.94) years. In contrary, at least half of the nurses were working in the current hospital and unit for less than five years with mean years of 5.26 (SD=3.67) and 4.26 (SD=3.02). The average number of weekly working hours at the hospital was 45.04 (SD=5.40) hours with the majority working not more than 48 hours per week. Continuous variables including age, number of service years, years of working in the current hospital and unit were categorized according to median cut-off respectively. Meanwhile, the self-reported BMI scored average value of 24.18 kg/m2 (SD=4.48) with approximately half of the nurses identified as normal.
Table 1 summarized the personal and occupational profiles of the studied nursing population. With regards to physical activities, using the SQUASH criteria, the nurses reported an overall weekly average time spent including commuting, working, household chores and leisure to be 3405.60 (SD=334.49) minutes per week. Three out of four nurses reported an average of 2521.17(SD=20.11) minutes per week dedicated for working whereas the least was spared for leisure activities (2.3%) and commuting (3.1%). Domestic activities represented 20% of overall allocated time. The distribution trend was observed to be almost similar with the results documented by the original author of SQUASH (Wendel-Vos, 2003), except for commuting (16%) and working (60%) on a study conducted among healthy participants. In addition, 53% of the total minutes of activity per week were spent in moderate intensity activities.
| Variables | % (n) | Mean (SD) | |
|---|---|---|---|
| Age (yrs.) | |||
| ≤30 | 53.70 (202) | 30.58 (5.25) | |
| >30 | 46.30 (174) | ||
| Years of employment as nurses (yrs.) | 7.38 (4.94) | ||
| ≤5 | 42.80 (161) | ||
| >5 | 57.20 (215) | ||
| Years working at the current hospital (yrs.) | 5.26(3.67) | ||
| ≤5 | 60.40(227) | ||
| >5 | 39.60(149) | ||
| 4.26(3.02) | |||
| Years working at the current unit (yrs.) | |||
| ≤5 | 68.90(259) | ||
| >5 | 31.10(117) | 45.04(5.40) | |
| Working hours/week (hrs.) | |||
| ≤48 | 85.90(323) | ||
| >48 | 13.80( 52) | ||
| Body Mass Index (BMI)(kg/m2) | 24.18(4.48) | ||
| Races | 94.10(354) | ||
| Malays | 5.90( 22) | ||
| Non-Malays | |||
| Marital status | 76.60 (288) | ||
| Married | 23.40 ( 88) | ||
| Not married | |||
| Level of education | 87.80 (330) | ||
| Tertiary (certificate/diploma/degree) | 12.20 ( 46) | ||
| Non-tertiary(lower and upper secondary) | |||
| Type of assigned ward | |||
| General/medical | 78.50(295) | ||
| Intensive care units | 21.50( 81) | ||
| Household income (MYR) | 3833.25(1536.73) | ||
| Physical activities (minutes per week) | |||
| Total score | 3400.22 (330.78) | ||
| Commuting | 104.46( 52.35) | ||
| Leisure activities | 77.15( 83.02) | ||
| Domestic activities | 699.52(300.98) | ||
| Activities at work | 2521.16 ( 20.08) | ||
Table 1: Characteristics of the studied nursing population (N=376)
Reliability of the Malay Translated Standardized Nordic Musculoskeletal Questionnaire
(M-SNMQ)
Reliability of the M-SNMQ test-retest survey was performed on 187 nurses using the Kappa agreement correlation coefficient as shown in Table 2. Overall, despite pain location, out of the 36 items of M-SNMQ, 21 items (58.3%) demonstrated an existence of strong kappa agreement values of at least 0.75. Among those, four items obtained a score equal to one, whilst the remaining 17 items illustrated a kappa value between 0.80 and 0.96. With regards to the individual study items and the annual prevalence question, all body regions scored a strong agreement of kappa coefficient values of at least 0.75. In comparison, only one item, weekly prevalence, scored an excellent value of 0.86, while the remaining items showed moderate agreement, valued between 0.54 and 0.69. The reliability of the test-retest method also assessed the kappa coefficient of the question regarding seeking professional healthcare assistance, which showed that 67% of the items indicated an excellent kappa agreement coefficient. In the present study, the question about the restriction in movement due to disorders yielded high nonagreement rates varying between 11% and 60%. Nonetheless, for elbows and thighs, the kappa coefficient values of two items namely: “prevention in the daily activities” and “seeking for physician assistance” could not be calculated because the nurses gave the same responses on both occasions.
| Body sites | During the past 12 months | During the last one month have you had trouble in: | ||
|---|---|---|---|---|
| Prevalence | Have you been prevented fromcarrying out normal activities | Have you seen a physician for this condition: | ||
| Neck | 0.80 | 0.80 | 1.00 | 0.60 |
| Shoulders | 0.90 | 0.66 | 0.56 | 0.86 |
| Upper back | 0.91 | 0.89 | 1.00 | 0.61 |
| Elbows | 0.96 | -* | -* | 0.66 |
| Wrists/hands | 0.82 | 0.95 | 0.95 | 0.60 |
| Lower back | 0.82 | 0.86 | 0.85 | 0.62 |
| Hips/thighs | 0.95 | -* | -* | 0.69 |
| Knees | 0.85 | 1.00 | 1.00 | 0.54 |
| Ankles/feet | 0.83 | 0.40 | 0.95 | 0.62 |
Table 2: The Kappa coefficient agreement of the studied items in M-SNMQ (N=187)
Prevalence of WRMSDs
Table 3 depicts the overall prevalence rates of WRMSDs of the studied population in the different body regions. The present study reveals that WRMSDs are widely experienced by the studied population with lifetime prevalence of 88.6%. Among those surveyed, majority of the nursing professionals agreed in their lifetime that the most common WRMSDs involved the feet (73.7%), neck (65.2%), shoulders (64.9%), and upper back (62.5%), while only 13.8% reporting symptoms in the arms or elbows. This study confirms that 73.1% of the nursing staff sustained WRMSDs symptoms in at least one anatomical site one year prior to the study. By the individual anatomical sites, 48.9% of the nurses reported the neck as the most common WRMSDs followed by feet/ankles (47.2%), upper back (40.7%), shoulders (37.0%), and lower back (35.3%) while the least complaint was observed in the arms/elbows (6.6%). At least two out of five nursing personnel sustained WRMSDs symptoms in five body regions for the past one month including neck, shoulders, upper back, lower back and ankles/feet, with the highest prevalence reported in the ankles/feet area (32.2%). A similar prevalence trend was also observed over the past seven days. Neck and ankles/feet were the most common sites for musculoskeletal symptoms experienced by the nurses (20.5%-21.3%), while less common sites involved the knees, thighs, wrists and arms.
| Body regions | Prevalence, % (n) | ||||||||
| Lifetime | 12-months | 1 month | 7-days | ||||||
| Neck | 65.2(245) | 48.9(184) | 59.2(109) | 21.3 (23) | |||||
| Shoulders | 64.9(244) | 36.9(139) | 59.0(82) | 13.1(11) | |||||
| Upper back | 62.5(235) | 40.7(153) | 55.6(85) | 14.4 (12) | |||||
| Arms/elbows | 13.8( 52) | 6.6 (25) | 28.0(7) | 1.3 ( 1) | |||||
| Wrists | 58.0(218) | 26.3 ( 99) | 47.5(47) | 6.9 ( 3) | |||||
| Lower back | 44.9(169) | 35.3(133) | 63.2(84) | 14.6 (12) | |||||
| Thighs | 34.6(130) | 19.4(73) | 53.4(39) | 5.6 (2) | |||||
| Knees | 47.9(180) | 25.6(96) | 61.5(59) | 8.5 (5) | |||||
| Ankles/Feet | 73.7(277) | 47.2(178) | 68.0(121) | 20.5 (25) | |||||
Table 3: Prevalence of WRMSD by anatomical site among nurses (N=376)
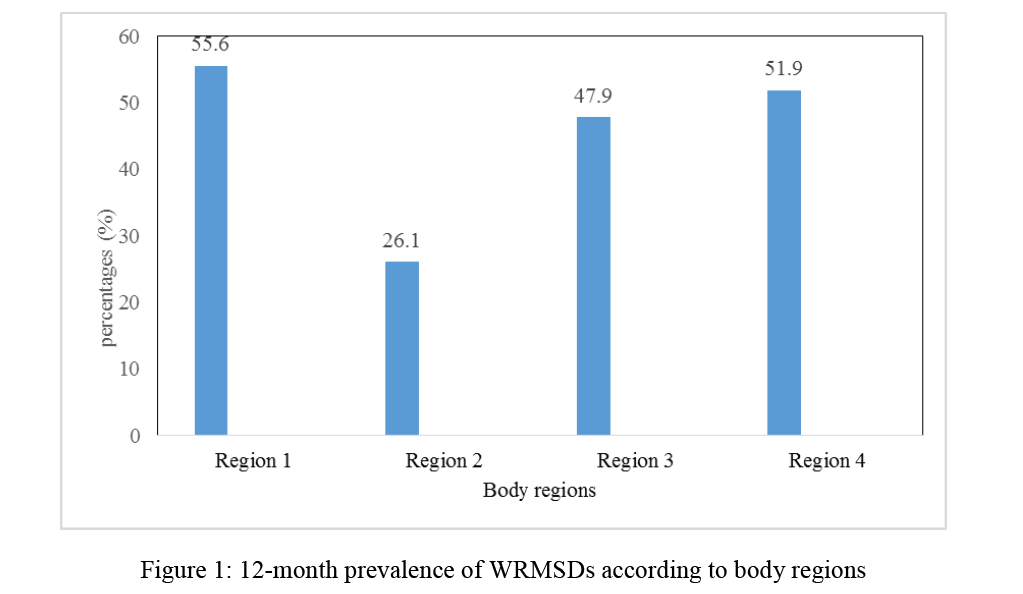
In order to extend statistical analysis further, the body regions were categorized into four anatomical regions; region 1 (neck and shoulders), region 2 (wrists, arms, and hands), region 3 (upper and lower back) and region 4 (thighs, knees, ankles, and feet). Over 50% of the nursing staff sustained WRMSD in region one (neck and shoulders) and region four (hips, knees, ankles, and feet), whereas only 26.1% nurses developed WRMSD in region two (wrists, arms and hands)(Figure 1). As seen in Figure 2, approximately 20% of the nursing personnel reported symptoms of WRMSDs in only one anatomical site. Over half of the nurses (54.8%) encountered musculoskeletal symptoms in multiple sites (≥2 sites) of body area over the last 12 months. Of these, only 8.2% and 10.4% experienced WRMSDs symptoms in two and three body regions, respectively.
The presence of WRMSDs in region 3 (upper and lower back) was strongly associated with the WRMSDs symptoms in region 4 (thighs, knees, ankles, and feet) (Φ=0.64, p<0.001). Whereas, the weakest association was reported between WRMSDs in region one (neck and shoulders) and region two (elbows, arms, wrists, and hands)(Φ=0.29, p<0.001). Moderate relationships were observed among other anatomical sites (Φ=0.40-0.56).
Impact of WRMSDs
Further investigations also showed that nurses with positive symptoms of WRMSDs at specific body regions faced the consequences of WRMSDs in their life (Table 4). Less than 10% admitted experiencing functional limitations in daily activities. Likewise, at least 80% of the affected nurses had never visited health professionals for medical treatment or were missing from work due to the disorders. In the previous one year, prevalence of absenteeism due to WRMSDs ranged from 6.2% to 18%. Among those, more nurses developing musculoskeletal symptoms in the shoulders (18%) and knees (17.7%) took medical leaves than those sustaining WRMSDs in other anatomical sites. The intensity of pain experienced by the nurses was assessed according to the definition by Bernard et al. (1994) [50]. Therefore, in the previous 12 months, the majority of the nursing personnel suffered from at least moderate pain or discomfort in the neck (83.2%), shoulders (72.7%) and ankles/feet (71.9%). Only 24% sustained at least moderate pain or discomfort in the arms area.
| Body site | No of individual developing WRMSD symptoms (n)+ | During the past 12 months, %(n) | |||||
|---|---|---|---|---|---|---|---|
| Affected daily activities# | Seeking for physician# | Taking medication# | Taking medical leave# | Suffered at least moderate pain (score ≥2) | |||
| Neck | 184 | 2.0 (4) | 10.0 (18) | 29.0 (53) | 13.6 (25) | 83.2 (153) | |
| Shoulders | 139 | 4.0 (6) | 7.2 (10) | 22.3 (31) | 18.0 (25) | 72.7 (101) | |
| Upper back | 153 | 5.9 (9) | 6.5 (10) | 22.2 (34) | 7.2 (11) | 58.2 ( 89) | |
| Arms | 25 | 4.0 (1) | 12.0 ( 3) | 8.0 ( 2) | 8.0 ( 2) | 24.0 ( 6) | |
| Wrists/hands | 99 | 7.1 (7) | 10.1 ( 9) | 17.2 (17) | 10.1 ( 9) | 40.4 ( 40) | |
| Lower back | 133 | 6.8 (9) | 9.0 (12) | 24.1 (32) | 12.0 (16) | 59.4 ( 79) | |
| Hips/thighs | 73 | 4.1 (3) | 2.7 ( 2) | 17.8 (13) | 9.6 ( 7) | 45.2 ( 33) | |
| Knees | 96 | 6.3 (6) | 5.2 ( 5) | 20.8 (20) | 17.7 (17) | 58.3 ( 56) | |
| Ankles/feet | 178 | 2.2 (4) | 4.5 ( 8) | 17.4 (31) | 6.2 (11) | 71.9 (123) | |
#% presented as a proportion of n
Table 4: Impact of WRMSDs and pain intensity among studied nursing population in the previous 12 months
Discussions
The occurrence of WRMSDs has become an occupational health concern worldwide [51]. Female workers were said to be more likely to sustain WRMSDs due to after-work responsibilities including parenting, undertaking domestic loads, insufficient rest time and lack of exercise [52]. Among healthcare workers, nurses were among the workers with high risks for WRMSDs because of their overwhelming burden of work [12,53–55].This study aimed to document the prevalence of self-perceived WRMSDs among nursing personnel working in public hospitals in Malaysia and also to evaluate the cross cultural adaptation of the M-SNMQ.
The SNMQ is internationally accepted as a screening instrument to assess the pain or discomfort of the musculoskeletal systems [47]. It was chosen to evaluate the WRMSDs among nursing personnel in this study following the majority of the earlier investigators [14,24,27]. The reliability of the instrument has been studied in the original version [47,56] as well as in the other foreign languages [57,58]. In the present study, the reliability of the M-SNMQ was assessed using Kappa agreement correlation coefficient. The reliability analyses found that over 50% of the studied items yielded strong kappa agreement values of at least 0.75 [49], majority scored kappa values at least 0.80 while remaining obtained values of 1. Of these, the question regarding the annual prevalence, all body regions scored a strong agreement of kappa coefficient values of at least 0.75 [49]. In comparison, only one item, weekly prevalence, scored an excellent value of 0.86, while the remaining items showed moderate agreement, valued between 0.54 to 0.69 [59]. This indicates that the respondents had better recalling of events in the preceding 12 months rather than other related questions. Therefore, corroborating a study by Marx et al. (2003) [60], which examined the length of time interval in the test-retest reliability, the current study illustrated no significant difference in the result obtained from the test-retest survey. This also shows that the time frame between the administrations of the questionnaires (3 months) does not affect the answer given by the respondents.
Further, the reliability of the test-retest method was also observed among those seeking for professional healthcare assistance with 67% of the items indicating excellent kappa reliability coefficient [49], in accordance with earlier studies [57-58,61]. Similarly, Rosecrance et al. (2002) [62] also reported generally acceptable values of kappa coefficient that varied between 0.40 and 0.82. In addition, the present findings were greater as compared to the outcome in the study from the original version of the SNMQ (0% to 23%) [47]. The question pertaining to about the restriction in movement due to disorders yielded high non-agreement rates varying between 11% to 60%, which is higher than discovered in the cross cultural study of SNMQ among a Brazilian population of less than 20% [57]. In agreement with findings in the previous international reliability study among a Portuguese population [58], the kappa coefficient values of two items: “prevention in the daily activities” and “seeking for physician assistance” for elbows and thighs could not be calculated because the nurses gave the same responses on both occasions. This could be explained due to the fact that the questionnaire was self-administrated; therefore the respondents intended to provide the worst answer. In addition, the nature of the response (binomial answer) had limited the respondents to express best answer. Nevertheless, the absence of these scores does not affect the overall assessment of WRMSDs in the present study. This reliability study is in synchronizing with a suggestion by Franzblau et al. (1997) [63], who encourages researchers to perform the study upon the use of musculoskeletal features as research instruments, therefore helping to improve occupational health research quality.
The prevalence rate of WRMSDs varied across occupational groups and over national boundaries [64] including nursing profession.18 A number of studies showed that among health professionals, the nursing personnel have the highest annual prevalence of WRMSDs [24,25]. The results of the current study indicated a lifetime prevalence of 88.6%.This is expected as most people encountered some degree of musculoskeletal pain in their lifetime [65,66]. The nursing population in our study reported a fairly high annual prevalence rate of 73.1% prior to the study, almost similar to the rates reported earlier [38,67]. In the past 12 months of this study, 48.9% of the studied nurses sustained WRMSDs symptoms in the neck, 47.2% (feet/ ankles), upper back (40.7%), shoulders (37%), and lower back (35.3%). Thighs and arms appeared to be the least pain and discomfort body areas of 19.4% and 6.6%, respectively. The prevalence rate of this study is slightly lower than those reported among nursing personnel who were surveyed using a similar research instrument (SNMQ) in previous epidemiological studies; the rates varied between 81% and 95% in Iran [15,26], Japan [16], Estonia [68] and Brazil [69]. Nonetheless, it was almost similar to the prevalence rates reported in other nursing population in the United States (72.5%) [23] and China (70.0%) [67]. Table 5 shows the comparison between the current study and other findings. The difference in prevalent rates and the ranking usually were explained by several possible factors such as different workplace settings [70] and the sociocultural [71]. For example, although the nurses’ tasks were homogenous, nurses working in intensive care units were more likely to sustain of WRMSDs in comparison to their peers in other units. This is due to the reasons that the patients were fully dependent and immobilize, hence more effort to be taken to take care of the patients [72]. In context of socio cultures, this was observed in a comparative study among Brazilian and Germany population, although using same technique and study instrument, German respondents reported higher prevalence [71].
| Country | Prevalence rate (%) | References |
|---|---|---|
| Malaysia | 73.1 | Current study |
| Iran | 95.0 | Mehrdad et al. (2010) |
| Brazil | 96.6 | Magnago et al. (2010) |
| China | 70.0 | Smith et al. (2004) |
| America | 75.0 | Trinkoff et al. (2002) |
| Korea | 93.6 | Smith et al. (2005) |
| Japan | 85.5 | Smith et al. (2006) |
| Estonia | 84.4 | Freimann et al. (2013) |
Table 5: Comparison of annual prevalence of WRMSDs among nursing personnel in the present and earlier studies
In the past 12 months, 48.9% of the studied nurses sustained WRMSDs symptoms in the neck, 47.2% (feet/ ankles), upper back (40.7%), shoulders (37%), and lower back (35.3%). Thighs and arms appeared to be the least painful and discomforting body areas (19.4% and 6.6%, respectively). Although the affected areas were similar, the ranking of location was slightly different than those reported in prior studies using the same research instrument (SNMQ) and technique (self-reported). Heiden et al. (2013) [73] and Mehrdad et al. (2010) [15] concluded that the lower back, neck, shoulders and knees were the most common problems faced by nursing professionals. The annual prevalence of neck pain among the studied nursing personnel showed higher than those recorded among western nurses74 and in a previous local study [75]. This was expected because nursing were exposed to the challenging working environment. In line, an earlier study by Hoe et al. (2012) [76] reported that workplace factors including lack of social support, high perceived workplace and high job strain were among the common factors associated with neck pain in Australian nursing workers. However, the rate was lower than those reported in previous investigations among other Asian counterparts (54.7% to 62.7%) [10,16].
Meanwhile, developing WRMSDs in the ankles or feet has affected more than one third of the studied nursing population for the past one year. The prevalence was comparatively lower than those reported in Australia (55.3%) [27] and Iran (59.0%) [24]. Nonetheless, a higher prevalence rate was observed in other international counterparts in Saudi Arabia (41.5%) [14] and China (34.4%) [67]. The nurses’ jobs required them to be in prolonged standing position and involved lots of walking. Although number of reasons can lead to development of WRMSDs in ankles and feet, but the most renowned reason is wearing inappropriate footwear that lack of support (such as high heels, thin insole) had increased the risk [77]. Although majority of the nurses presenting the ankles/feet symptoms sustained moderate pain, less than 5% of the nurses agreed that having WRMSDs in ankles/feet has a pervasive impact in their quality of life, in contrary with previous nursing study (16.7%) [27].
Next, the third most frequently reported WRMSDs was in the upper back (40.7%). It was in a considerable range observed among nursing personnel in Japan (33.9%) [16] and Korea (38.8%) [10]. More than one third of the nursing personnel, developed the WRMSDs symptoms in the shoulders area in agreement with the Greek [78] and Egyptian [79] nursing personnel. Although the existing literature documented the lower back as a commonly affected area among nursing staffs, our study revealed quite different findings. Low Back Pain (LBP) was in the fifth row with annual prevalence of 35.3% similar to those in Ugandan nursing staffs [11]. The prevalence was much lower than reported in earlier studies in England (45%) [55], Japan (71.3%) [16], Australia (63%) [80] and Sweden (50.3%-64.0%) [20,8]. As compared to other local studies [21,81], our findings demonstrated lower prevalence in LBP (35.3%). This may reflect by the type of hospital settings, in which our study took place in tertiary hospitals while the aforementioned studies were done in district hospitals. The tertiary hospitals were well equipped with mechanical lifting aides and also had higher number of staffs, hence, reduced the workloads of the nurses. The musculoskeletal symptoms were less prevalent in the arms (6.6%), similarly demonstrated among Nigerian nurses (7.7%) [38]. Whereas in the other reports, a higher prevalence rate between 10% and 17.9% were observed among Chinese67 and Iranian nurses [6]. However, musculoskeletal symptoms in the elbows or arms were significant among Malaysian women despite being different in racial groups [82].
In addition, for the previous one year to this study, approximately 20% of the studied nurses complained of symptoms of WRMSDs in only one anatomical site that were lower than those reported among American nurses (35%) [83]. Meanwhile, over half of the participants (54.8%) encountered WRMSDs in the multisite (≥2 sites) of body area over the last 12 months, closely corresponding to the Estonian nurses (60%) [68]. Of the percentage, not more than 10% reported of WRMSDs in two and three body regions respectively. The findings were much lower than compiled in the previous epidemiological studies between 15.8% to 50% respectively [83,84]. Thus, it is convinced that multi-site pain or discomfort of the musculoskeletal system is a common health problem observed among nursing personnel [48,84,85]. Over 40% of the nurses affected by the WRMSDs in five body regions for the past one month include neck, shoulders, upper back, lower back and ankles/feet, with the highest prevalence observed in the ankles/feet area of 32.2%. Coggon et al. (2013) [86], in The Cultural and Psychosocial Influences on Disability (CUPID) survey, discovered higher one-month prevalence rates varying between 37.7% to 42.6% among nursing personnel in Costa Rica and Nicaragua. In agreement, Daraiseh et al. (2010) [48] also demonstrated relatively higher one-month prevalence in similar anatomical sites of the neck (55.2%), shoulders (50.0%), lower back (74.1%), and ankles/feet (52.5%). In another study in Japan, it was discovered that a greater prevalence of WRMSDs in the lower back and shoulders was between 42.8% to 54.7% respectively [87]. On the other hand, less than 10% of the nurses reported WRMSDs in the arms/elbows or thighs similarly observed in Sri Lankan nursing personnel [12]. Earlier, Surawera et al. (2012) [88] found that Australian nursing personnel had a higher prevalence rate of WRMSDs at 15.3% in the wrist or hand.
The same prevalence rate was also documented for the past seven days prior to the research. Over 20% of the nurses sustained WRMSDs in the neck and ankles/feet, respectively, whilst the lowest prevalence of WRMSDs were documented in the knees, thighs, wrists and arms areas. These findings were slightly higher than those reported by Reed et al. (2014) [27], except for the ankles/feet (16.8%) among Australian nurses. Likewise, a study conducted among Portuguese employees also recorded low prevalence across body regions except in the upper back regions (35%) [58]. However, Sorour & El-Maksoud (2012) [79] also discovered that less than 10% of the studied Egyptian nurses reported pain or related WRMSDs in the wrists’ area for the past one week before the study. In another study by Josephson et al. (1997) [8], it was documented that a higher seven days prevalence rate of 69% for neck, shoulders, lower and upper back among Swedish nurses.
The present study also showed that for the past 12 months, majority of the nurses suffered from at least moderate pain or discomfort in the neck, shoulders and ankles/feet areas as compared to the arms. Using the same case definition, the present study reported a higher prevalence rate in comparison to other female dominated occupations, such as flight attendants (31%-54%) [89] and nurses (22%-32%) [23]. Less than 10% of the nurses admitted that the WRMSDs had limited their daily activities consistent with Widanarko et al. (2014) [28]. Nonetheless, a study conducted among nurses in Germany discovered that over 20% nurses developing WRMSDs in the feet and lower back agreed that the disorders had disturbed their norms activities [73]. Smith et al.(2005) [10], in their findings described that approximately half of the Korean nurses have denied that WRMSDs has affected their daily routine.
Similarly, less than 20% of the nurses visited healthcare professionals for treatment. These rates appeared to be lower than in other studies. This might have reflects the level of awareness of the studied nurses. In the prior local study, Veerapen et al.(2007) [82] reported that at least two out of five Malaysians developing musculoskeletal symptoms will seek for treatment either from modern or traditional practitioners. On the other hand, over 50% of healthcare workers developing musculoskeletal symptoms either in the back, neck or shoulders sought for treatment, hence, reflecting that the American nurses were more concerned on their health [23]. In the current study, the prevalence of absenteeism due to WRMSDs ranged between 6.2% to 18%, with more nurses developing WRMSDs in the neck, knees and shoulders taking medical leave than those sustaining the WRMSDs in other anatomical sites. On the contrary, Engels et al. (1996) [19] reported that 40% of the Dutch’s nurses with back pain took sickness absences more frequent than their peers with arms or neck pain. Nonetheless, the statistics is slightly higher than found in the CUPID study conducted in Japan, which less than 5% of Japanese workers were reported taking medical leave due to the pain related to the musculoskeletal system [90]. Meanwhile, under the same project, less than 10% of the workers in New Zealand have absented from work due to developing symptoms of WRMSDs in the arms, wrists, neck and shoulders [28].
Conclusion
The study has addressed some possible limitations. Firstly, as the data was obtained from a cross sectional study, the results should be interpreted with caution because it does not imply its causality. Secondly, the data were collected using self-reported techniques; participant responses may be biased as a result of social desirability to provide sociably preferred answers than the real experiences [91]. In congruent with Silverstein et al. (1997) [92], after examined data obtained from a variety of sources, it concluded that greater prevalence rate of WRMSDs were reported using self-administered than using pre-existing medical history. Thirdly since the present study was limited to the female nursing personnel and working in shift, the obtained data may have not represented the overall prevalence among nursing personnel. Hence, future study shall also recruited male nursing personnel and those working in non-shift schedule.
Despite its limitation, as compared to other local studies which focused on particular body areas, our study offers new knowledge on the prevalence patterns of WRMSDs (lifetime, annual, monthly, seven days) across body regions and also the impacts of WRMSDs to the nurses [21,81]. Results of the present study indicates that WRMSDs were common occupational health problems among nurses in Malaysia, similarly, observed in other studies. Nonetheless, the findings also correspond with the perception that the nurses may have considered WRMSDs as common illnesses due to the nature of their jobs [93]. This are reflects through the low percentages on reports of WRMSDs related impacts such as medical seeking behaviour and also absenteeism rate. Additionally, the present study also indicates good reliability of test-retest methods hence, suggested that the M-SNMQ is a reliable instrument to assess the symptoms of musculoskeletal of the nursing population. Future study is required to identify the associated potential risk factors, thus providing sufficient information to the stakeholders to reduce the risk.
Funding
This study was funded by Jeffrey Cheah School of Medicine and Health Sciences, Monash University Malaysia and the University of Kuala Lumpur.
Ethics approval
The study received ethics approval from the Monash University Human Research Ethics Committee (MUHREC)(CF12/506-2012000809) and Ministry of Health, Malaysia Research Ethics Committee (MREC)(NMRR-12-234-11176).
Conflict of interest
The authors declare that they have no conflict of interest.
Acknowledgements
The authors would like to acknowledge, with gratitude we appreciate the support from the Ministry of Health, Malaysia for granting the permission to conduct this study. Special thanks to the Chief Matrons and also nursing staffs from four hospitals in the Klang Valley area for their valuable participations.
References
- Nordin NAM, Leonard JH, Thye NC. Work-related injuries among physiotherapists in public hospitals: A Southeast Asian picture. Clinics. 2011;66(3):373-378. doi:10.1590/S1807- 59322011000300002.
- Lee LK, Ismail NH. Implication of the Prevalence of Needlestick Injuries in a General Hospital in Malaysia and Its Risk in Clinical Practice. Environ Health Prev Med. 2005;10:33-41. doi:10.1265/ehpm.10.33.
- Centre for Disease Control and Prevention. National Occupational Research Agenda for Musculoskeletal Disorders. Cincinnati: National Institute for Occupational Safety andHealth; 2001.
- European Agency for Safety and Health at Work. Work-Related Musculoskeletal Disorders: Back to Work Report. Luxembourg; 2007.
- United States Bureau of Labor statistics. Nonfatal Occupational Injuries and Illness Requiring Days Away from Work.; 2013. www.bls.gov/news.release/pdf/osh2.pdf.
- Choobineh, A, Rajaeefard,A, Neghab M. Association Between Perceived Demands and Musculoskeletal Disorders Among Hospital Nurses of Shiraz University of Medical Sciences: A Questionnaire Survey. Int J Occup Saf Ergon. 2006;12(4):409-416.
- Engkvist, I., Hagberg, M., Hjelm, E.W. Menckel, E, Ekenvall L. Risk Indicators for Reported Over-Exertion Back Injuries among Female Nursing Personnel. Epidemiology. 2000;11(5):519-522.
- Josephson M, Lagerstrom M, Hagberg M, Hjelm EW. Musculoskeletal symptoms and job strain among nursing personnel?: a study over a three year period. Occup Environ Med. 1997;54:681-685.
- Lipscomb JA, Trinkoff AM, Brady B, Geiger-Brown J. Health care system changes and reported musculoskeletal disorders among registered nurses. Am J Public Health. 2004;94(8):1431-1435.
- Smith DR, Choe MA, Jeon MY, Chae YR, An GJ, Jeong JS. Epidemiology of musculoskeletal symptoms among Korean hospital nurses. Int J Occup Saf Ergon. 2005;11(4):431-440.
- Munabi IG, Buwembo W, Kitara DL, Ochieng J, Mwaka ES. Musculoskeletal disorder risk factors among nursing professionals in low resource settings: a cross-sectional study in Uganda. BMC Nurs. 2014;13:7. doi:10.1186/1472-6955-13-7.
- Warnakulasuriya SSP, Peiris-John RJ, Coggon D, Ntani G, Sathiakumar N, Wickremasinghe AR. Musculoskeletal pain in four occupational populations in Sri Lanka. Occup Med (Lond). 2012;62(4):269-272. doi:10.1093/occmed/kqs057.
- Anap D, Iyer C, Rao K. Work related musculoskeletal disorders among hospital nurses in rural Maharashtra, India?: A multi centre survey. Int J Res Med Sci. 2013;1(2):101-107. doi:10.5455/2320-6012.ijrms20130513.
- Attar SM. Frequency and risk factors of musculoskeletal pain in nurses at a tertiary centre in Jeddah, Saudi Arabia: a cross sectional study. BMC Res Notes. 2014;7(1):61. doi:10.1186/1756-0500-7-61.
- Mehrdad R, Dennerlein JT, Haghigat, M. & Aminian O. Association Between Psychosocial Factors and Musculoskeletal Symptoms Among Iranian Nurses. Am J Ind Med. 2010;53(10):1032-1039. doi:10.1002/ajim.20869.
- Smith DR, Mihashi M, Adachi Y, Koga H, Ishitake T. A detailed analysis of musculoskeletal disorder risk factors among Japanese nurses. J Safety Res. 2006;37(2):195-200. doi:10.1016/j.jsr.2006.01.004.
- Smith DR, Wei N, Kang L, Wang R-S. Musculoskeletal disorders among professional nurses in mainland China. J Prof Nurs. 2004;20(6):390-395. doi:10.1016/j.profnurs.2004.08.002.
- Alexopoulos EC, Burdorf ÆA, Kalokerinou A. A comparative analysis on musculoskeletal disorders between Greek and Dutch nursing personnel. Int Arch Occup Environ Health. 2006;79(1):82-88. doi:10.1007/s00420-005-0033-z.
- Engels JA, Gulden, JWJ. van der G, Senden, TF, van’t Hof B. Work Related Risk Factors for Musculoskeletal Complaints in the Nursing Profession?: Results of a Questionnaire Survey. Occup Environ Med. 1996;53(9):636-641.
- Fochsen G, Josephson M, Hagberg M, Toomingas A, Lagerstrom M. Predictors of leaving nursing care: a longitudinal study among Swedish nursing personnel. Occup Environ Med. 2006;63(3):198-201. doi:10.1136/oem.2005.021956.
- Rahmah, MA, Rosy, J, Halim, I, Jamsiah, M, Shamsul A. Prevalence of Back Pian among nurses working in government health clinicis and Hospital in Port Dickson Malaysia. J Community Health. 2008;14(2):11-18.
- Yip VYB. A study of work stress , patient handling activities and the risk of low back pain among nurses in Hong Kong. J Adv Nurs. 2001;36(6):794-804.
- Trinkoff AM, Lipscomb JA, Geiger-brown J, Brady B. Musculoskeletal Problems of the Neck , Shoulder , and Back and Functional Consequences in Nurses. Am J Ind Med. 2002;41:170-178. doi:10.1002/ajim.10048.
- Choobineh, A, Movahed, M, Tabatabaie, SH, Kumashiro M. Perceived Demands and Musculoskeletal Disorders. Ind Health. 2010;48:74-84.
- Trinkoff AM, Lipscomb JA, Geiger-Brown J, Storr CL, Brady BA. Perceived physical demands and reported musculoskeletal problems in registered nurses. Am J Prev Med. 2003;24(3):270-275. doi:10.1016/S0749-3797(02)00639-6.
- Abedini R, Choobineh A, Hasanzadeh J. Musculoskeletal Load Assessment in Hospital Nurses with Patient Transfer Activity. Int J Occup Hyg. 2008;5(2):39-45.
- Reed LF, Battistutta D, Young J, Newman B. Prevalence and risk factors for foot and ankle musculoskeletal disorders experienced by nurses. BMC Musculoskelet Disord. 2014;15(1):196. doi:10.1186/1471-2474-15-196.
- Widanarko B, Legg S, Devereux J, Stevenson M. The combined effect of physical, psychosocial/organisational and/or environmental risk factors on the presence of work-related musculoskeletal symptoms and its consequences. Appl Ergon. 2014;45(6):1610-1621. doi:10.1016/j.apergo.2014.05.018.
- Buckle, P & Devereux J. The nature of work-related neck and upper limb musculoskeletal disorders. Appl Ergon. 2002;33:207-217.
- Piedrahita H. Costs of work-related musculoskeletal disorders (MSDs) in developing countries: Colombia case. Int J Occup Saf Ergon. 2006;12(4):379-386.
- Industry Commision. Work, Health and Safety: An Inquiry into Occupational Health and Safety. Report No 47(Vol 2). Vol 2. Canberra, Australia: Commonwealth of Australia;1995.
- International Labour Organizational. Estimating the Economic Costs of Occupational Injuries and Illnesses in Developing Countries?: Essential Information for Decision-Makers. Geneva: International Labour Office; 2012. https://www.ilo.org/safework/info/publications.
- ILO International Financial and Actuarial Service?; ILO Regional Office for Asia and the Pacific?; Social Security Organization. Malaysia?: Report to the Social Security Organization on the Ninth Actuarial Valuation. Geneva, Switzerland: InternationalLabourOrganization; 2013.
- Australian Safety and Compensation Council. Occupational Exposures of Australian Nurses: Results of the Project. Australia; 2008.
- Widanarko B, Legg S, Stevenson M, et al. Prevalence and work-related risk factors for reduced activities and absenteeism due to low back symptoms. Appl Ergon. 2012;43(4):727-737. doi:10.1016/j.apergo.2011.11.004.
- Department of Occupational Safety and Health Malaysia. Annual Report 2012. Kuala Lumpur; 2012.
- Daniel WW. Biostatistics: A Foundation for Analysis in the Health Sciences. New York: John Wiley & Sons. Inc.; 1999.
- Tinubu BMS, Mbada CE, Oyeyemi AL, Fabunmi AA. Work-related musculoskeletal disorders among nurses in Ibadan, South-west Nigeria: a cross-sectional survey. BMC Musculoskelet Disord. 2010;11(12):1-8. doi:10.1186/1471-2474-11-12.
- Roth P., Fred SS, Switzer DM. Missing Data in Multiple Item Scales?: A Monte Carlo Analysis of Missing Data Techniques. Organ Res Methods. 1999;2(3):211-232.
- Fauziah, N, Quek, KF, Agus Salim MB. Relationship between nature of work and psychosocial among nurses working in Hospital Selayang, Selangor. Malaysian J Public Heal Med. 2006;6(2):56-61.
- Chang AM, Bedst M, Dipned H, Frcna RN. Translation of questionnaires and issues of equivalence. J Adv Nurs. 1999;29(2):316-322.
- Jones, EG & Kay M. Instrumentation in Cross Cultural Research. Nurs Res. 1992;41(3):186-188.
- Wendel-Vos GCW. Reproducibility and relative validity of the short questionnaire to assess health-enhancing physical activity. J Clin Epidemiol. 2003;56(12):1163-1169. doi:10.1016/S0895-4356(03)00220-8.
- Ainsworth, BE, Haskell, WL, Leon, AS, et al. Conpedium of Physical Activies: A second updates of codes and MET values. Med Sci Sports Exerc. 2011;43(8):1575-1581.
- Berkel J Van, Proper KI, Dam A Van, Boot CRL, Bongers PM, Beek AJ Van Der. An exploratory study of associations of physical activity with mental health and work engagement. BMC Public Health. 2013;13:558-564. doi:10.1186/1471-2458-13-558.
- Wagenmakers R, van den Akker-Scheek I, Groothoff JW, et al. Reliability and validity of the short questionnaire to assess health-enhancing physical activity (SQUASH) in patients after total hip arthroplasty. BMC Musculoskelet Disord. 2008;9:141. doi:10.1186/1471-2474-9-141.
- Kuorinka I, Jonsson B, Kilbom A, et al. Standardised Nordic questionnaires for the analysis of musculoskeletal symptoms. Appl Ergon. 1987;18(3):233-237.
- Daraiseh NM, Cronin SN, Davis LS, Shell RL, Karwowski W. Low back symptoms among hospital nurses, associations to individual factors and pain in multiple body regions. Int J Ind Ergon. 2010;40(1):19-24. doi:10.1016/j.ergon.2009.11.004.
- Fleiss JL. Statistical Methods for Rates and Proportions. 2nd Editio. New York: John Willey & Sons; 1981.
- Bernard BP, Sauter S, Fine L, et al. Job task and psychosocial risk factors for work-related musculoskeletal disorders among newspaper employees. Scand J Work Environ Health. 1994;20(6):417-426.
- National Research Council & Institute of Medicine. Musculoskleletal Disorders and the Workplace: Low Back and Upper Extremeties. Washington, DC: National Academy Press;2001.
- Strazdins L & Bammer G. Women, work and musculoskeletal health. Soc Sci Med. 2004;58(6):997-1005. doi:10.1016/S0277-9536(03)00260-0.
- Harcombe H, Herbison GP, McBride D, Derrett S. Musculoskeletal disorders among nurses compared with two other occupational groups. Occup Med (Chic Ill). 2014;64(8):601-607. doi:10.1093/occmed/kqu117.
- National Institute for Occupational Safety and Health. Musculoskeletal Disorders and Workplace Factors. Bernard BP (Ed.). Cincinnati: National Institute for OccupationalSafety and Health; 1997.
- Smedley J, Egger P, Cooper C, Coggon D. Manual handling activities and risk of low back pain in nurses. Occup Environ Med. 1995;52(3):160-163.
- Dickinson CE, Campion K, Foster AF et al. Questionnaire development: an examination of the Nordic Musculoskeletal questionnaire. Appl Ergon. 1992;23(3):197-201.
- de Barros ENC, Alexandre NMC. Cross-cultural adaptation of the Nordic musculoskeletal questionnaire. Int Nurs Rev. 2003;50(2):101-108.
- Mesquita CC, Ribeiro JC, Moreira P. Portuguese version of the standardized Nordic musculoskeletal questionnaire: cross cultural and reliability. J Public Health (Bangkok). 2010;18(5):461-466. doi:10.1007/s10389-010-0331-0.
- Cohen J. A Coefficient of Agreement for Nominal Scales. Educ Psychol Meas. 1960;20(1):37-46. doi:10.1177/001316446002000104.
- Marx RG, Menezes A, Horovitz L, Jones EC, Warren RF. A comparison of two time intervals for test-retest reliability of health status instruments. J Clin Epidemiol. 2003;56(8):730-735. doi:10.1016/S0895-4356(03)00084-2.
- Dawson AP, Steele EJ, Hodges PW, Stewart S. Development and test-retest reliability of an extended version of the Nordic Musculoskeletal Questionnaire (NMQ-E): a screening instrument for musculoskeletal pain. J Pain. 2009;10(5):517-526. doi:10.1016/j.jpain.2008.11.008.
- Rosecrance JC, Ketchen KJ, Merlino LA et al. Test-Retest Reliability of a Self-Administered Musculoskeletal Symptoms and Job Factors Questionnaire Used in Ergonomics Research. Appl Occup Environ Hyg. 2002;17(9):613-621. doi:10.1080/1047322029009593.
- Franzblau A, Salerno D, Armstrong T, Werner R. Test-retest of an upper extremity discomfort reliability questionnaire in an industrial population. Scand J Work Environ Health. 1997;23(4):299-307.
- Smith DR, Kondo N, Tanaka E et al. Musculoskeletal disorders among hospital nurses in rural Japan. Rural Remote Health. 2003;3(3):241.
- Widanarko B, Legg S, Stevenson M, et al. Prevalence of musculoskeletal symptoms in relation to gender , age , and occupational / industrial group. Int J Ind Ergon. 2011;41(5):561-572. doi:10.1016/j.ergon.2011.06.002.
- Wijnhoven H, de Vet HCW, Picavet HSJ. Prevalence of musculoskeletal disorders is systematically higher in women than in men. Clin J Pain. 2006;22(8):717-724. doi:10.1097/01.ajp.0000210912.95664.53.
- Smith DR. Musculoskeletal complaints and psychosocial risk factors among Chinese hospital nurses. Occup Med (Lond). 2004;54(8):579-582.
- Freimann T, Coggon D, Merisalu E, Animagi L, Paasuke M. Risk factors for musculoskeletal pain amongst nurses in Estonia: a cross-sectional study. BMC Musculoskelet Disord. 2013;14:334. doi:10.1186/1471-2474-14-334.
- Magnago TSB, Lisboa MTL, Griep RH, Kirchhof ALC, De Azevedo Guido L. Psychosocial aspects of work and musculoskeletal disorders in nursing workers. Rev Lat Am Enfermagem. 2010;18(3):429-435.
- Harcombe H, McBride D, Derrett S, Gray A. Physical and psychosocial risk factors for musculoskeletal disorders in New Zealand nurses, postal workers and office workers. Inj Prev. 2010;16:96-100. doi:10.1136/ip.2009.021766.
- Raspe H, Matthis C, Croft P, O’Neill T. Variation in back pain between countries: the example of Britain and Germany. Spine (Phila Pa 1976). 2004;29(9):1017-1021; discussion 1021. doi:10.1097/00007632-200405010-00013.
- Ovayolu, O, Ovayolu, N, Genc,M, Nilgun, CA. Frequency and severity of low back pain in nurses working in intensive care units and influential factors. Pakistan J Med Sci. 2014;30(1):70-76.
- Heiden B, Weigl M, Angerer P, Müller A. Association of age and physical job demands with musculoskeletal disorders in nurses. Appl Ergon. 2013;44(4):652-658. doi:10.1016/j.apergo.2013.01.001.
- Lipscomb JA, Trinkoff AM, Geiger-Brown J, Brady B. Work-schedule characteristics and reported musculoskeletal disorders of registered nurses. Scand J Work Environ Health. 2002;28(6):394-401. doi:10.5271/sjweh.691.
- Alshagga MA, Nimmer AR, Yan LP et al. Prevalence and factors associated with neck , shoulder and low back pains among medical students in a Malaysian Medical College. BMC Res Notes. 2013;6:244-250. doi:10.1186/1756-0500-6-244.
- Hoe VCW, Kelsall HL, Urquhart DM, Sim MR. Risk factors for musculoskeletal symptoms of the neck or shoulder alone or neck and shoulder among hospital nurses. Occup Environ Med. 2012;69(3):198-204. doi:10.1136/oemed-2011-100302.
- Riskowski, J, Dufour, AB, & Hannan M. Arthritis, Foot pain & Shoe wear: Current musculoskeletal research on feet. Curr Opin Rheumatol. 2011;23(2):148-155. doi:10.1097/BOR.0b013e3283422cf5.Arthritis.
- Alexopoulos EC, Burdorf A, Kalokerinou A. Risk factors for musculoskeletal disorders among nursing personnel in Greek hospitals. Int Arch Occup Environ Health. 2003;76(4):289-294. doi:10.1007/s00420-003-0442-9.
- Sorour AS, El-Maksoud MMA. Relationship between musculoskeletal disorders, job demands, and burnout among emergency nurses. Adv Emerg Nurs J. 2012;34(3):272-282. doi:10.1097/TME.0b013e31826211e1.
- Lusted MJ, Carrasco CL, Mandryk JA, Healey S. Self reported symptoms in the neck and upper limbs in nurses. Appl Ergon. 1996;27(6):381-387.
- Wong T, Teo N, Kyaw M. Prevalence and Risk Factors Associated with Low Back Pain Among Health Care Providers in a District Hospital. Malaysian Orthop J. 2010;4(2):23-28 doi:10.5704/MOJ.1007.004.
- Veerapen K, Wigley RD, Valkenburg H. Musculoskeletal Pain in Malaysia?: A COPCORD Survey. J Rheumatol. 2007;34(1):207-213.
- Daraiseh NM, Genaidy A, Karwowski W, Davis LS, Stambough J&, Huston RI. Musculoskeletal outcomes in multiple body regions and work effects among nurses: the effects of stressful and stimulating working conditions. Ergonomics. 2003;46(12):1178-1199. doi:10.1080/0014013031000139509.
- Sembajwe G, Tveito TH, Hopcia K, et al. Psychosocial stress and multi-site musculoskeletal pain: a cross-sectional survey of patient care workers. Workplace Health Saf. 2013;61(3):117-125. doi:10.3928/21650799-20130226-01.
- Lagerstrom M, Wenemark M, Hagberg M, Hjelm EW. Occupational and individual factors related to musculoskeletal symptoms in five body regions among Swedish nursing personnel. Int Arch Occup Environ Health. 1995;68(1):27-35.
- Coggon D, Ntani G, Palmer KT, et al. Disabling musculoskeletal pain in working populations: is it the job, the person, or the culture? Pain. 2013;154(6):856-863. doi:10.1016/j.pain.2013.02.008.
- Ando S, Ono Y, Shimaoka M, et al. Associations of self estimated workloads with musculoskeletal symptoms among hospital nurses. Occup Environ Med. 2000;57(3):211-216.
- Surawera IK, Hoe VCW, Kelsall HL, Urquhart DM, Sim MR. Physical and psychosocial factors associated with wrist or hand pain among Australian hospital-based nurses. Inj Prev. 2013;19:13-18. doi:10.1136/injuryprev-2011-040267.
- Lee H, Wilbur J, Kim MJ, Miller AM. Psychosocial risk factors for work-related musculoskeletal disorders of the lower-back among long-haul international female flight attendants. J Adv Nurs. 2008;61(5):492-502. doi:10.1111/j.1365-2648.2007.04511.x.
- Matsudaira K, Palmer KT, Reading I, Hirai M, Yoshimura N, Coggon D. Prevalence and correlates of regional pain and associated disability in Japanese workers. Occup Environ Med. 2011;68(3):191-196. doi:10.1136/oem.2009.053645.
- Cook C. Mode of administration bias. J Man Manip Ther. 2010;18(2):61-63. doi:10.1179/106698110X12640740712617.
- Silverstein, BA, Stetson, DS, Koeyserling, WM, Fine L. Work-related musculoskeletal disorders: comparison of data sources for surveillance. Am J Ind Med. 1997;31:600-608.
- Retsas A, Pinikahana J. Manual handling activities and injuries among nurses: an Australian hospital study. J Adv Nurs. 2000;31(4):875-883.
Open Access Journals
- Aquaculture & Veterinary Science
- Chemistry & Chemical Sciences
- Clinical Sciences
- Engineering
- General Science
- Genetics & Molecular Biology
- Health Care & Nursing
- Immunology & Microbiology
- Materials Science
- Mathematics & Physics
- Medical Sciences
- Neurology & Psychiatry
- Oncology & Cancer Science
- Pharmaceutical Sciences